39 Spinal Cord Injury
 Epidemiology
Epidemiology
Spinal cord injury typically occurs in males at the peak of their productive lives. The incidence of traumatic SCI is approximately 11,000 new cases each year in the United States,1 with a prevalence of 191,000. The prevalence of SCI patients is increasing steadily owing to improved survival in both the acute and chronic stages of the disease. The amount spent on the treatment of spinal cord injuries in the United States is approximately 5.6 billion dollars each year and rising annually.2 The cost of caring for the individual spinal cord–injured patient is directly related to the injury level of the spinal cord and to the patient’s age, with the highest costs associated with older quadriplegic patients who are dependent on a ventilator.2
 Etiology
Etiology
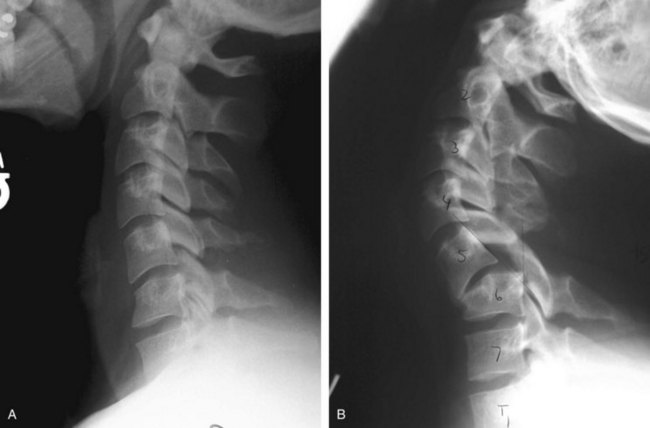
Most spinal injuries result from high-speed motor vehicle accidents (Figure 39-1). Falls and work-related injuries are other important contributors. Spinal cord injury that is due to violence is on a dramatic rise secondary to increased incidence of assaults. These injuries include both blunt and penetrating injuries, such as gun and knife wounds. Sports-related injuries, which include football, horseback riding, and hockey injuries, are relatively rare but have received recent media attention.3–4 Finally, recreational injuries from jet skis, snowmobiles, snow skiing, snowboarding, and parachuting, to name but a few, appear to be on the rise as “extreme sports” become more prevalent.
 Immobilization and Diagnostic Evaluation
Immobilization and Diagnostic Evaluation
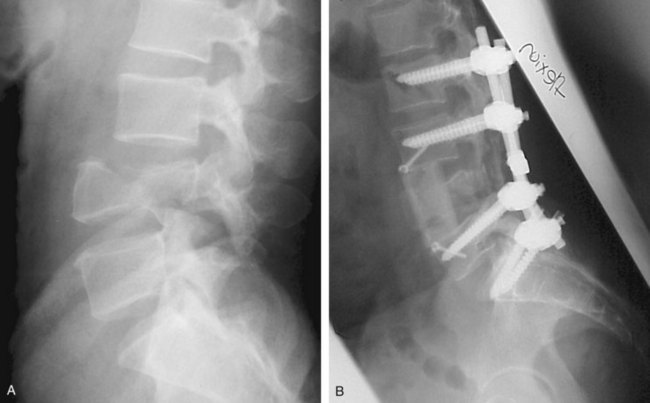
Further diagnostic studies will be dictated by the findings of the initial and secondary surveys as well as findings of initial diagnostic studies. Several points are important to keep in mind. First, important information can be obtained from studies performed for other reasons. For example, routine chest and abdominal radiographs may provide important information regarding the presence of significant thoracic/lumbar spine injury. Although these do not replace subsequent “formal” spine studies, they are often obtained as part of the routine trauma workup and provide early clues to the presence of spine trauma and may help prioritize subsequent imaging studies (Figure 39-2). Radiographs and particularly the CT are the most sensitive tools in detecting a fracture of the spine, but occasionally it is difficult to clear the spine—even in the absence of a fracture—because an unstable ligamentous injury without fracture may exist.
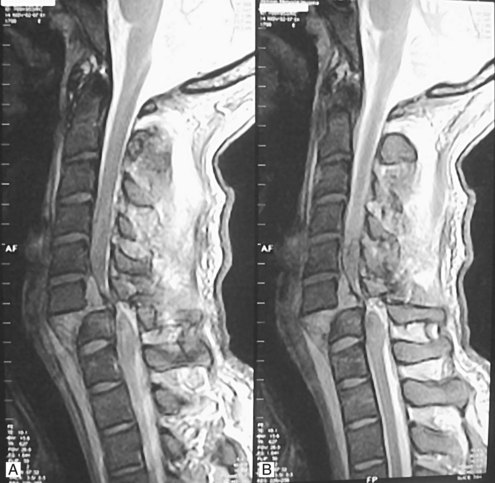
Patients with a suspected spinal column injury who are unconscious, uncooperative, or intoxicated or who have associated traumatic injuries that distract from their assessment will often require further radiographic study of the cervical spine before the discontinuation of cervical spine immobilization. Several options exist and include (1) maintenance of the collar and/or spine precautions until the patient becomes coherent and responsive, (2) dynamic imaging of the spine with physician monitoring, and (3) magnetic resonance imaging (MRI) of the spine to rule out a purely ligamentous injury. Of the three options, we frequently use MRI to clear the spine because a completely negative MR image in the setting of trauma indicates that there is no instability of the cervical spine (Figure 39-3). Malalignment and evidence of spine trauma on these imaging studies frequently determines subsequent management and diagnostic decision making. Cervical subluxations often require the use of traction and/or manual reduction of the fracture-dislocation. Diazepam (Valium) or lorazepam (Ativan), along with careful neurologic monitoring, often in the intensive care unit (ICU) setting, is required because application of traction can realign the spine but can also result in neurologic deterioration.
 Pediatric Spinal Cord Injury
Pediatric Spinal Cord Injury
Pediatric spine trauma is relatively uncommon, representing approximately 5% of all spinal cord injuries.5 For a specific discussion of pediatric SCI, please see Chapter 210. In addition, guidelines have been published on this topic.6
 Pharmacotherapy
Pharmacotherapy
The concepts of primary and secondary SCI are important principles in understanding the pathophysiology and the role of pharmacotherapeutic agents in emergent treatment. The primary injury mechanism results from a mechanical insult that occurs at the time of impact and includes acute compression, impaction, distraction, laceration, and shear.7 Secondary injuries occur after the initial injury and account for some of the progressive pathologic changes associated with SCI.7 A number of drugs have been tested in the laboratory, but only a few of these agents have progressed to clinical trials to evaluate their efficacy. Five randomized controlled trials of pharmacotherapy for acute SCI have been conducted, focusing on the therapeutic effect of either corticosteroids or gangliosides.
Corticosteroids
A number of studies have shown improved neurologic recovery in animals with spinal cord injuries that have received either dexamethasone or methylprednisolone.8–12 Corticosteroid treatment initially held promise as a potential therapeutic agent for its putative role in reducing white matter edema and inflammation. Current evidence, however, suggests that the major mechanism of action is reduction of the effects of secondary injury—in particular, the destructive effects of lipid peroxidation on cell membranes.2 Other actions include improving spinal cord blood flow, enhancing the postinjury activity of Na+/K+-ATPase, and facilitating the recovery of extracellular calcium ion.8,13
The first NASCIS trial (NASCIS I) examined low- (100 mg) and high- (1000 mg) dose methylprednisolone given for 10 days. Unfortunately, this trial had no control group, and no significant difference in outcome was found except for an increased number of wound infections among patients in the high-dose group.14 The second NASCIS trial (NASCIS II) was a prospective, randomized, double-blind, multicenter trial that demonstrated improved neurologic outcomes after 6 weeks, 6 months, and 1 year in patients with nonpenetrating SCI who had received a regimen of methylprednisolone, which included a bolus dose of 30 mg/kg.15 Improvement in motor and sensory scores associated with administration of methylprednisolone was only observed if the drug was given within 8 hours of injury when compared with naloxone or a placebo. Results of this study have been criticized.16,17 Some of the criticisms relate to difficulties in randomization, reporting methods, analysis of benefit limited to small subgroups within the larger study, and lack of replication of results by a completely independent group of investigators, among others. However, the administration of methylprednisolone is believed to reduce the amount of secondary injury that occurs after SCI and has become an important tool in the treatment of SCI in most North American centers. The results of NASCIS III have been published and compared the dosage of methylprednisolone used in the NASCIS II protocol with a longer dosing regimen (48 hours) as well as with a 21-aminosteroid. The 21-aminosteroids (lazaroids), a new class of steroids that are potent inhibitors of lipid peroxidation, lack much of the glucocorticoid activity of many of the traditional steroid compounds. Results of the study suggested that when patients are seen within 3 hours of their injury, they should receive a bolus dose of methylprednisolone (30 mg/kg intravenously [IV]) followed by 23 hours of treatment (5.4 mg/kg/h IV). Patients seen between 3 and 8 hours should receive the same bolus followed by a longer dosing regimen (48 hours). Complications from 48 hours of treatment included a significant increase in severe sepsis and pneumonia.18 Neurosurgical guidelines for management of spine trauma recommend methylprednisolone as a treatment option, recognizing that the risks of use have been more clearly demonstrated than benefit.19,20
Gangliosides
Gangliosides are complex sialic acid–containing glycosphingolipids which are present in high concentrations in neural membranes. These compounds are involved in a variety of cell-surface phenomena such as cell-substrate binding and receptor functions.21 Basic research in the past 15 years has demonstrated that these compounds can (1) promote the survival of neurons in cell culture; (2) increase the number, length, and branching of neuronal processes in cell culture; and (3) improve functional recovery after a variety of traumatic and ischemic insults to the peripheral and central nervous system. A limited number of animal studies have examined the role of gangliosides after SCI and have shown only a modest effect on the regeneration of serotonergic neurons.22 A recent prospective, randomized, double-blind, single-center study found a beneficial effect in functional neurologic outcomes when the ganglioside GM1 was administered within 72 hours of human SCI.23 However, a multicenter trial demonstrated no statistically significant benefit with administration of this agent at 26 and 52 weeks after injury.24
 Hypothermia
Hypothermia
Two recent studies were published on the safety and feasibility of mild to moderate intravascular cooling for SCI. Levi et al. reported on a series of 14 patients with American Spinal Injury Association (ASIA) classification A complete cervical cord injuries who underwent a protocol to achieve temperatures of 33.5°C via a closed-loop delivery system. Researchers found good correlation between intravascular and intrathecal cerebrospinal fluid temperature.25 Average time between inductions of hypothermia was 9.17 ± 2.24 hours (mean ± SEM); time to target temperature was 2.72 ± 0.42 hours; duration of cooling at target was 47.6 ± 3.1 hours; and average total length of time of cooling was 93.6 ± 4 hours. A subsequent paper summarized the complications and neurologic outcomes seen in the SCI patients treated with hypothermia and compared them to age- and injury-matched controls. The hypothermia group ASIA conversion rate to a higher grade was approximately 42%, with a similar frequency of complications to institutional controls.26 This pilot study suggested that systemic intravascular cooling can be accomplished with minimal variations in temperature and few adverse events, and may pave the way for larger multicenter SCI trials to test the efficacy of mild to moderate hypothermia in SCI.27
 Intensive Care Unit Management
Intensive Care Unit Management
Spinal cord injury is associated with profound effects on all vital systemic functions. Through primarily class III medical evidence, numerous reports indicate lower morbidity and mortality rates in patients with SCI managed with ICU monitoring and aggressive medical management of these changes.28–36 At the least, these studies taken together indicate that a systematic approach must be taken to evaluate and treat each of the potential complications. Early and late complications will be seen, and the degree of involvement of each system is usually correlated with the level and severity of injury.
Respiratory System
Respiratory complications are a major source of morbidity and mortality after SCI, with an 18% to 30% mortality rate reported in patients with tetraplegia.32,37 In a study by Hachen and associates,28,30 most early deaths were related to pulmonary complications, with the likelihood of severe insufficiency related to SCI severity. Whereas most cervical spinal cord injuries occur below C4, with the phrenic nerves continuing to innervate the diaphragm, the respiratory system is frequently severely affected, particularly after cervical spinal cord injuries. Specifically, marked reductions in (forced) vital capacity, inspiratory capacity, and expiratory flow rates frequently result in hypoxemia.28,32,38–41 These changes may be attributed to variable paralysis of the intercostal muscles and accessory muscles of respiration. Loss of abdominal muscle tone and ileus also reduce the mechanical efficiency of breathing.
The most common respiratory complications include atelectasis, pneumonia, pulmonary embolus, pulmonary edema, and acute respiratory distress syndrome. In addition to difficulty with taking deep breaths and coughing, patients are often unable to clear airway secretions. Accumulation of secretions and/or mucus plugs can result in respiratory failure. Prevention includes respiratory treatment with bronchodilators, frequent pulmonary toilet, chest physiotherapy, increasing airway humidity, intubation, and mechanical ventilation including the use of continuous positive airway pressure. The use of the RotoRest bed significantly decreases pulmonary complications associated with SCI32,42 because it improves pulmonary blood flow and reduces the incidence of pulmonary emboli.
Most patients can be discontinued or weaned from the ventilator after they have been medically stabilized, which usually means treatment of pulmonary infections, reestablishment of euvolemia, enhancement of respiratory muscle function, and nutritional supplementation to offset the high caloric requirements of the trauma. Initially, weaning the intermittent mandatory ventilation rate is followed by weaning of the positive airway pressure (either continuous or end-expiratory). With prolonged periods of ventilation (>2 weeks), and/or multiple failed extubations, one should consider a tracheostomy. The likelihood of requiring a tracheostomy increases after a high SCI, preexisting pulmonary disease, and the age of the patient. Tracheostomy effectively reduces the physiologic dead space. Northrup and colleagues43 have demonstrated that a tracheostomy can be performed before anterior cervical instrumentation of the spine, with a low risk of infection; but in our patient population, early surgery for stabilization is advocated, and consequently, few patients undergo tracheostomy before anterior cervical stabilization surgery.

Full access? Get Clinical Tree