a. Decreased maternal O2 tension is an uncommon cause of intrapartum fetal asphyxia. Clinical situations that may result in decreased maternal O2 tension and fetal hypoxia include anemia, pulmonary edema, smoking, maternal apnea, pulmonary embolus, severe asthma, cyanotic heart disease, and amniotic fluid embolus. High altitude is another cause of decreased maternal O2 tension.
b. Interrupted umbilical blood flow prevents O2 delivery from the placenta to the fetus. When the umbilical cord is occluded (e.g., cord prolapse), fetal afterload increases, initiating a vagal response that produces fetal bradycardia. If the occlusion is intermittent in an otherwise healthy fetus, the bradycardia may become intermittent in the form of variable decelerations.
c. Inadequate uterine blood flow results in impaired fetal O2 uptake. Uterine blood flow is not autoregulated and is a major determinant of O2 delivery across the placenta. Because uteroplacental perfusion is proportionate to blood pressure (BP), reduction below a certain threshold results in inadequate fetal O2 uptake. Examples of acute reductions in uterine blood flow include hypotension associated with neuraxial anesthesia or abruptio placentae. Uteroplacental insufficiency produced by hypertensive disorders (e.g., preeclampsia) is an example of chronic insufficiency. Intermittent reductions in blood flow can also result from maternal supine positioning secondary to aortocaval compression and uterine contractions.
d. Fetal pathology is an uncommon cause of fetal asphyxia. Examples include (1) fetus with increased metabolic rate (e.g., pyrexia) or (2) decreased O2 carrying capacity (e.g., anemia).
CLINICAL PEARL The overall incidence of neonatal encephalopathy attributable to intrapartum hypoxia in the absence of any other preconception or antepartum abnormalities is estimated to be approximately 1.6 per 10,000.
2. Fetal acid–base balance and asphyxia. The umbilical artery cord blood pH, PaO2, PacO2, and the calculated base excess are the most objective determinations of the fetal metabolic condition at the time of delivery.8 However, the definitions of normal umbilical cord blood gases and base deficit is unclear because vigorous infant with Apgar scores >7 at 5 minutes can be born with umbilical arterial pH of <7.1 with base excess of 11 mEq per L. During asphyxia, there is a continuum of decreasing PaO2, accompanied by increasing PacO2, and decreasing pH. Despite the low PaO2, tissues continue to consume O2. In the presence of very low PaO2, anaerobic metabolism results, producing metabolic acidosis. This is partially buffered by bicarbonate in the blood.
If fetal hypoxia occurs just before birth, there may be lactic acid in the tissues that has not yet reached the central circulation. The diagnosis of intrapartum fetal asphyxia requires a blood gas and acid–base assessment. The important question for the clinician is what is the threshold of metabolic acidosis beyond which fetal morbidity or mortality may occur.8
3. Fetal response to asphyxia. Fetal anoxia evolves at varying rates, and severe asphyxia can be lethal in <10 minutes.9 It is clinically important to realize that fetal cardiac output is maintained early in asphyxia, but its distribution changes markedly as the process progresses. The healthy term fetus is able to mount a series of compensatory mechanisms that protect the brain from hypoxia-related damage. Fetal cerebral metabolic responses to acute hypoxia include reducing energy consumption, increasing oxygen extraction, and maximizing substrate delivery.10 During the advanced stages of asphyxia, O2 delivery to the brain and heart decreases and the myocardium consumes glycogen reserves. Evolving lactic acidosis and the progressively lower PaO2 and pH lead to myocardial dysfunction and redistribution of blood flow to vital organs. Generally, myocardial failure does not occur until both pH and PaO2 are extremely low, approximately 6.9 and 20 mm Hg, respectively. Although human studies make it clear that an isolated severe hypoxic–ischemic insult can lead directly to fetal brain injury, they also suggest that this is a rare event and that many cases of encephalopathy are associated with preceding or coexisting factors.11 The difference between a hypoxic insult that leads to fetal/neonatal death versus that causing significant fetal stress with a normal long-term neurologic outcome is probably very small.
B. Diagnosis
1. Fetal heart rate monitoring was introduced over four decades ago, but the interpretation and management of FHR patterns during labor remains one of the most problematic issues in obstetrics. FHR monitoring is one of the few tools available for assessing fetal status and oxygenation during labor and delivery. The relative merits of FHR monitoring have nevertheless been the subject of substantial debate. Central to the conflict are issues regarding interpretation, reproducibility of interpretation, and management of abnormal patterns. Disappointing outcomes associated with electronic FHR monitoring may be related to the observations that many cases of asphyxial damage begin before labor and intrapartum FHR monitoring will not detect antepartum events that would otherwise prompt intrapartum interventions. Fetal and neonatal outcomes are not improved with the use of continuous electronic FHR monitoring compared to intermittent FHR electronic auscultation.12 The incidence of cerebral palsy has not decreased in the last 30 years!
a. Fetal heart rate pattern. Because of the lack of agreement about pattern interpretation as well as the high number of false-positive tracings, a Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) consensus panel in 2008 proposed a uniform system of terminology in which any FHR pattern is classified as category I, II, or III, based on the presence or absence of well-defined aspects of the FHR.13 With this in mind, subsequent recommendations have been developed by the ACOG for the management of category I (normal) and category III (pathologically abnormal) FHR patterns. The management of category II FHR patterns remains the most important and challenging issue in the field of FHR monitoring, but recommendations regarding the clinical management have been developed.14
b. Interpretation of fetal heart rate. It is generally accepted that decreased baseline FHR variability is the single most reliable predictor of fetal compromise. During asphyxia, FHR variability decreases and then disappears before significant fetal depression or death occurs in utero. Decreased variability correlates clinically with decreased central nervous system (CNS) function and is thought to precede CNS damage. In cases where variability is absent and/or the FHR is persistently <80 beats per minute (bpm) (category III), there is no time to reduce fetal stress and immediate delivery is indicated. Patients with category II (all FHR patterns not classified as category I or III) tracings should be evaluated for factors that may reduce fetal oxygenation but most importantly take into account associated clinical circumstances.
CLINICAL PEARL Fetal and neonatal outcomes are not improved with the use of continuous electronic FHR monitoring compared to intermittent FHR electronic auscultation.
2. Presence of meconium
Meconium staining has often been associated with neonatal depression. In a recent prospective cohort study, the presence of meconium was associated with higher risk of the composite morbidity.15 However, in most cases, the finding is not of serious importance because it is not necessarily indicative of intrauterine asphyxia. Historically, the presence of meconium-stained amniotic fluid during labor was a potentially ominous sign, but controversy exists over its relative impact on fetal status. Data indicate that timing and quantity of meconium passage are critical variables for assessing the significance of this occurrence on fetal well-being. Presumably, these two aspects of meconium passage correlate with the duration and severity of the intrauterine insult. If meconium staining is present in combination with an abnormal FHR tracing or another risk factor (e.g., intrauterine growth restriction [IUGR], postdates), there is an increased likelihood of neonatal depression. More important, aspiration of meconium-stained fluid can lead to serious neonatal morbidity and mortality.
CLINICAL PEARL In most cases of meconium staining, the finding is not of serious importance because it is not necessarily indicative of intrauterine asphyxia.
3. Umbilical cord gases
a. American College of Obstetricians and Gynecologists recommendation for umbilical cord blood gas sampling. The determination of pH, blood gases, and base deficit in umbilical cord blood is commonly performed to assess the metabolic status of the newborn in conjunction with Apgar scores and the neonatal clinical course. In 2006, ACOG recommended selective sampling only if a serious abnormality arises in the delivery process or a problem occurs in the newborn period.8 Fetal acidemia is often considered a sign of more permanent neonatal morbidity and is used as an indicator of risk for adverse neonatal outcome. Although the degree of asphyxia can be determined by the extent of acidemia, it does not necessarily reflect the duration of the insult.
b. Umbilical cord gas limits. Previously, a normal umbilical cord pH was at least 7.2. However, these limits have been challenged because they do not distinguish between differences in arterial and venous blood samples. These limits have been challenged even further by differences in blood samples obtained following labor as well as those obtained from premature infant deliveries. For example, if a fetus has been subjected to the stress of labor, acidemia should be defined as an umbilical artery pH <7.15 or an umbilical vein pH <7.2. By definition, acidemia refers to increased hydrogen ion concentration in the blood. Acidosis occurs when there is increased hydrogen ion concentration in the tissues. Asphyxia includes both hypoxia (i.e., decreased pO2 in tissues) as well as CO2 retention. The combination of these may lead to acidosis. However, in most cases, the term birth asphyxia should be avoided because there are no precise clinical or biochemical indicators that have a high positive predictive value for perinatal asphyxia.
CLINICAL PEARL In most cases, the term birth asphyxia should be avoided because there are no precise clinical or biochemical indicators that have a high positive predictive value for perinatal asphyxia.
4. Doppler ultrasound
Doppler ultrasound is used to assess blood flow in the fetal arterial and venous systems. It is as an important tool used in antenatal surveillance for the management and timing of delivery in pregnancies associated with IUGR. Evaluation of the umbilical arteries provides information on placental resistance. Placental resistance is elevated in uteroplacental insufficiency. This leads to a reduction in forward umbilical artery flow and is reflected by a relative reduction in diastolic as compared to systolic velocities. Absent or reversed end diastolic flow in the umbilical artery is known to be associated with an 80-fold increased risk of perinatal mortality.16 Neonatal intracranial volume and cerebral cortical gray matter, as measured by magnetic resonance imaging (MRI), were also reduced in infants born from pregnancies complicated by fetal growth restriction and abnormal umbilical artery Doppler studies compared with matched infants of the same gestational age but with appropriate intrauterine growth.17
The measurement of blood flow velocities in umbilical and fetal cerebral arteries is a valuable tool in antepartum surveillance.
CLINICAL PEARL The ideal time for delivery is when abnormalities exist only in the umbilical and venous circulations and before abnormalities are observed in the FHR tracing. However, this may be influenced by gestational age.
C. Treatment
1. Obstetric management
Type II and type III FHR patterns warrant active medical intervention. When there is an unresolved, prolonged severe bradycardia (class III FHR pattern), emergency cesarean delivery (CD) will be necessary to minimize fetal risk. The management of a class II FHR pattern will depend on the presence or absence of moderate variability or accelerations, the response of the FHR to contractions and the progress and stage of labor. With a category II FHR pattern, several maneuvers can be utilized to resuscitate the fetus in utero (see Table 16.2). Fetal O2 content and saturation can be improved by administering supplemental O2 and by placing the mother in the left lateral position to reduce compression of the vena cava. Uterine stimulants (i.e., oxytocin infusion) should also be discontinued. Tocolysis should be considered to achieve uterine relaxation if the mother is hemodynamically stable and there is no evidence of abruptio placentae. Terbutaline, 0.25 mg administered subcutaneously (SQ) or intravenously (IV) has been found to be superior to placebo and to magnesium sulfate in relieving decelerations. Sublingual nitroglycerin spray can achieve more rapid uterine relaxation, but its use may cause hypotension and maternal headache. IV hydration should be considered if the volume status is in question. Maternal hypotension resulting from neuraxial anesthesia should also be corrected. A vaginal examination should be performed to rule out rapid cervical change and fetal descent as well as cord prolapse. If there is evidence of cord compression by the presence of repetitive, moderate to severe variable decelerations, amnioinfusion should be considered. If the FHR abnormalities do not resolve with the earlier mentioned measures, CD or operative vaginal delivery is indicated. Maternal fever can lead to increased fetal oxygen consumption and is associated with increased risk of poorer neonatal outcome. Treatment with acetaminophen and cooling measures should be instituted.

CLINICAL PEARL Anesthetic considerations for category II FHR patterns include administration of supplemental O2, left uterine displacement, IV hydration, correction of hypotension resulting from neuraxial anesthesia, treating uterine overstimulation, and preparation for cesarean or operative vaginal delivery.
2. Anesthetic management
Anesthesia for CD of a distressed fetus must provide proper operating conditions for the obstetrician within a short time period without compromising maternal or fetal safety. The obstetrician determines the timing and speed with which the procedure must be performed. The choice of general, spinal, or extension of an existing epidural anesthetic depends on the clinical circumstances. Although general anesthesia (GA) may be indicated in some cases of FHR abnormality, the severity of the abnormality should be considered before incurring risk associated with GA.18
a. Interpretation of the 30-minute rule
Clinicians have attempted to provide guidance on the time frame when an emergent CD should be initiated. In 1982, ACOG proposed a 15-minute interval between the time of decision for a CD to its start. These guidelines, however, were revised in 1989, and the 15-minute recommendation was extended to 30 minutes.19
A 30-minute interval is reported to be adequate for most CD. The Optimal Goals for Anesthesia Care in Obstetrics emphasize the “Availability of anesthesia and surgical personnel to permit the start of a cesarean delivery within 30 minutes of the decision to perform the procedure”20; in cases of vaginal birth after cesarean (VBAC), appropriate facilities and personnel, including obstetric anesthesia, nursing personnel, and a physician capable of monitoring labor and performing CD, immediately available during active labor to perform emergency CD. “The definition of immediate availability of personnel and facilities remains a local decision, based on each institution’s available resources and geographic location.”20 Although there are early reports of evidence for increased risk of fetal loss if the “alarm to surgery” interval exceeds 20 minutes21 and another report suggested that permanent fetal CNS damage may begin after approximately 10 minutes of fetal anoxia,22 most cases of fetal asphyxia are not the result of fetal anoxia. In cases where complete fetal anoxia is suspected, delivery should occur as soon as possible. Because these emergencies may occur at any time, the anesthesia provider must always be prepared for emergent operative delivery.
CLINICAL PEARL “Availability of anesthesia and surgical personnel to permit the start of a cesarean delivery within 30 minutes of the decision to perform the procedure”; in cases of VBAC, appropriate facilities and personnel, including obstetric anesthesia, nursing personnel, and a physician capable of monitoring labor and performing CD, immediately available during active labor to perform emergency CD. “The definition of immediate availability of personnel and facilities remains a local decision, based on each institution’s available resources and geographic location.”20
b. Anesthetic choice
Every woman admitted to labor and delivery has the potential to develop an obstetric emergency as a result of nonreassuring fetal status. When choosing an anesthetic, the anesthesia provider must communicate with the obstetrician to determine the urgency of the situation. “A communication system should be in place to encourage early and ongoing contact between obstetric providers, anesthesiologists, and other members of the multidisciplinary team.”23
Because most anesthesiologists and other anesthesia providers are not experts in FHR monitoring, it is up to the obstetrician to determine the severity of the FHR abnormality. Emergency CD is performed when the situation is life threatening for either the mother or fetus. In cases of abnormal FHR patterns, emergency CD is indicated for prolonged fetal bradycardia, late decelerations without FHR variability, and cord prolapse with bradycardia.
“The decision to use a particular anesthetic technique for cesarean delivery should be individualized, based on several factors. These include anesthetic, obstetric, or fetal risk factors (e.g., elective vs. emergency), the preferences of the patient, and the judgment of the anesthesiologist. Neuraxial techniques are preferred to GA for most cesarean deliveries. An indwelling epidural catheter may provide equivalent onset of anesthesia compared to initiation of spinal anesthesia for urgent cesarean delivery. . . . However, GA may be the most appropriate choice in some circumstances (e.g., profound fetal bradycardia, ruptured uterus, severe hemorrhage, severe placental abruption)”23 but the risk of a difficult airway (and availability of backup and advanced airway equipment) should always be considered.
CLINICAL PEARL The obstetrician determines the severity of the FHR abnormality. Emergency CD is performed when the situation is life threatening for either the mother or fetus. Neuraxial techniques are preferred to GA for most CD.
(1) Local anesthetics and fetal acidosis
The use of 2% lidocaine with or without epinephrine may be associated with fetal ion trapping of the local anesthetic in the presence of severe fetal acidosis. The balance of ionized and nonionized forms of a local anesthetic is shifted toward the ionized, poorly lipid-soluble form in the acidotic environment. This imbalance has led many investigators to believe that local anesthetics (in particular, lidocaine) may accumulate in the acidotic environment. Despite this theoretical concern, pH adjusted 2% lidocaine with epinephrine is commonly used in practice. In some situations, 3% 2-chloroprocaine can be used because it is almost completely hydrolyzed by maternal plasma esterases before it reaches the fetal circulation.
c. Maternal safety
Complications related to anesthesia remain an important and often preventable cause of obstetric-related mortality. Although maternal mortality has declined significantly in the last 50 years, the rate of decline stabilized from 1980 to 2000. The most recent report from the Centers of Disease Control and Prevention indicates that pregnancy-related deaths in the United States have steadily increased from 7.2 deaths per 100,000 live births in 1987 to a high of 17.8 deaths per 100,000 live births in 2009 and 2011.24 Although the reasons for the overall increase in pregnancy-related deaths are unclear, numbers of pregnant women with chronic diseases (hypertension, obesity, diabetes, chronic heart disease) are increasing and likely contributory to the increased mortality rates.
Anesthesia-related maternal mortality in the United States is estimated at 1.7 per 1,000,000 live births.25 During the 1970s and 1980s, 17 women died as a result of GA for every one that died from neuraxial anesthesia. By the early 1990s, this had improved to six GA deaths for every neuraxial anesthetic death. More recently, the serious complication repository project of the Society for Obstetric Anesthesia and Perinatology captured data on more than 250,000 anesthetics, including 3,000 general anesthetics.26 Although serious complications occurred in only 1:3,000 obstetric anesthetics, high neuraxial block, respiratory arrest in labor and delivery, and unrecognized spinal catheters were the most frequent complications identified. Leading causes of death were hemorrhage and preexisting cardiac disease. Another recent report of maternal deaths at a tertiary care center identified hypertensive disease and thromboembolic events as the leading causes of death. Access to a tertiary care center (distance of residence to the hospital) appeared to be the primary factor associated with maternal deaths.27 Despite advances in obstetric and anesthesia care, catastrophic complications do occur. These reports further emphasize the need for clear communication between obstetrician, anesthesia providers, and nursing staff as well as implementation of a “disaster” plan.
II.Peripartum bleeding
Obstetric emergencies contribute significantly to maternal morbidity and mortality. In a review of closed anesthesia malpractice claims, obstetric hemorrhage accounted for more than 30% of the hemorrhage claims, and lapses in communication contributed to 60% of the cases. Recent developments in the management of medical emergencies emphasize the value of a protocol-based team approach and regular simulation-based rehearsal of the management algorithms.28
A. Management of obstetric hemorrhage
1. Fundamentals of obstetric hemorrhage
Hemorrhagic shock is a condition in which inadequate perfusion of organs results in insufficient availability of O2 to satisfy the metabolic needs of the tissues. A catabolic state develops. The consequences of these changes are inflammation, endothelial dysfunction, and disruption of normal metabolic processes in vital organs. The initial assessment of the patient with blood loss requires only basic clinical evaluations. Monitoring of BP, pulse, capillary refill, mental status, and urinary output is sufficient to judge the amount and the rate of blood loss and to plan therapy. Scrupulous attention to these indices is important because visual estimates of obstetric blood loss are notoriously unreliable, and the failure to recognize early signs of hypovolemia can lead to irretrievable complications. Pregnant patients tolerate blood loss of up to 15% of their blood volume (approximately 1 L in a 70 kg woman at term) without symptoms or alterations in vital signs. When blood loss exceeds about 1,500 mL, hemodynamic changes (e.g., tachycardia, hypotension) begin to occur (see Table 16.3).
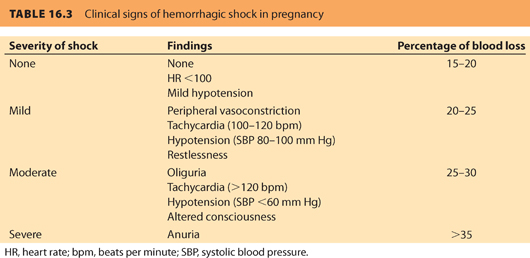
Tachycardia develops, often with a narrowing of pulse pressure; systolic blood pressure (SBP) may remain normal. Capillary refill may also be delayed. At this point, the patient often becomes anxious. Failure to recognize anxiety and restlessness in a postoperative or postpartum patient as early signs of hypoperfusion is a common error with potentially fatal consequences. As blood loss continues, tachypnea develops and urine output falls substantially. If untreated, the patient’s restlessness progresses to confusion. With massive losses (>3,000 mL), the pulse is often >140 bpm, BP is markedly decreased, capillary refill absent, and marked oliguria develops. The patient becomes lethargic and, eventually, comatose.29 The Joint Commission30 and the Society of Maternal Fetal Medicine recommended the adoption of protocols to address maternal death and morbidity that are associated with postpartum hemorrhage (PPH).28 Within a large health care system, the application of a standardized method to address maternal hemorrhage significantly reduced maternal morbidity, based on the need for maternal transfusion and peripartum hysterectomy.31
2. Key management considerations include
a. Hypotension is a late sign of hypovolemia because of the increased blood volume associated with pregnancy. Obstetric blood loss is often underestimated. Blood loss can be underestimated by 50% with the reliability of visual estimation decreasing as blood loss increases.32 Visual aids can be used to objectively and subjectively improve estimation of blood loss.33 Ongoing blood loss should be addressed without delay.
b. Because of the risk of considerable blood loss, large bore IV access should be obtained early during resuscitative efforts.
c. Either crystalloid or colloid can be used to assist in restoring blood volume because an atonic uterus can lose up to 2 L of blood in 5 minutes. In addition, more than 1 L of blood can be sequestered in an atonic uterus. This degree of blood loss occurs because nearly 15% of the cardiac output perfuses the uterus at term. Because pregnancy expands blood volume, hemorrhage may go undetected until the patient becomes hypotensive and tachycardic.
d. An arterial line is often useful for beat-to-beat monitoring of the BP and for obtaining hemoglobin, blood gases, and coagulation studies.
e. Anesthesia providers should for transfusion of blood products. If the institution has a massive transfusion protocol, it should be activated when there is substantial blood loss. If coagulopathy is likely, it is prudent to give blood products before coagulation studies deteriorate.
f. If medical interventions fail, other interventions may be necessary including intrauterine balloon (or gauze) tamponade and uterine compression sutures. Next steps include radiologic embolization or pelvic devascularization. Hysterectomy is reserved for refractory cases.
3. Transfusion in obstetric hemorrhage
The ASA Practice Guidelines for Obstetric Anesthesia state that a routine blood cross match is not necessary for vaginal or operative delivery. The decision whether to order or require a blood type and screen, or cross match, should be based on maternal history, anticipated hemorrhagic complications (e.g., placenta accreta in a patient with placenta previa and previous uterine surgery), and local institutional policies.23 In addition, the ASA Task Force on Obstetric Anesthesia and the ACOG recommend that all facilities providing obstetric care be prepared to manage hemorrhagic emergencies.23,34 Response to hemorrhage takes a coordinated effort between clinicians and the blood bank. It is helpful to have a massive hemorrhage protocol outline before an emergency occurs. Facilities should also consider writing and posting such a protocol in addition to initiating clinical drills on obstetric hemorrhage scenarios.31
4. Transfusion thresholds: when to transfuse
Determining the point when a parturient should be transfused is often difficult because blood loss during and after delivery is often underestimated. In these situations, blood loss arises from several areas and amniotic fluid is also present. Vital signs, ongoing hemorrhage, and coexisting disease should be considered. Signs and symptoms of inadequate perfusion resulting from hypovolemia include tachycardia, decreased pulse pressure, tachypnea, decreased urine output, and altered mental status. Although the physiologic changes of pregnancy help mitigate the parturient’s response to hemorrhage and vital signs may not change until more than 1,500 mL of blood loss has occurred, patients should be transfused when there are signs of significant hypoperfusion.
The purpose of packed red blood cell (PRBC) administration is to increase the O2 carrying capacity of blood. In the past, the goal of transfusion therapy was a hemoglobin concentration of 10 g per dL. Recently, this threshold was challenged by a study reporting decreased mortality rates in critically ill patients who were transfused at lower thresholds (<7 g per dL).35 However, in obstetric patients, Karpati et al.36 reported an approximately 50% incidence of myocardial ischemia in the intensive care unit (ICU) patients who were admitted with a diagnosis of PPH and hypovolemic shock. Risk factors for myocardial ischemia in these patients included a hemoglobin concentration of ≤6.0 g per dL, SBP ≤88 mm Hg, diastolic BP ≤50 mm Hg, and a heart rate (HR) >115 bpm. Interestingly, a recent survey of anesthesiologists and obstetricians determined that the transfusion threshold for PRBCs for most providers was between 7.0 and 8.0 g per dL with anesthesiologists transfusing at a lower threshold (i.e., 7.5 g per dL) compared to obstetricians (i.e., 8.0 g per dL).37 The ASA Task Force on Blood Replacement has concluded that PRBC administration is rarely indicated when the hemoglobin concentration is >10 g per dL but is almost always indicated when the hemoglobin level is ≤6 g per dL.38 In some centers, an arterial blood gas is used to guide transfusion therapy. If the base deficit is >15 mEq per L, in the presence of significant and ongoing blood loss, then blood should be administered.
5. Antepartum donation/autologous transfusion
Obstetric cases receive approximately 5% of blood components used annually throughout the United States. One potential method for reducing the need for homologous blood transfusions is autologous transfusion of the patient’s donated blood. Normally, blood center programs schedule donors once per week for up to 6 weeks preceding surgery. In some cases, erythropoietin is administered before surgery in an attempt to reduce the amount of homologous blood transfused. Unfortunately, with few exceptions, the results are disappointing. Most trials of erythropoietin given prior to surgery do not result in reduction of homologous blood transfused, although most have documented a positive impact on reticulocyte count and preoperative hematocrit.39
Routine autologous blood donation is not utilized for routine obstetric deliveries because of concern about cost-effectiveness.40 However, it is a reasonable option for patients at risk for peripartum hemorrhage, especially those with rare antibodies who may be difficult to transfuse with compatible homologous blood. Autologous donation during pregnancy has been shown to have minimal maternal hemodynamic effects.
Yamada et al.41 published an analysis of 82 patients with placenta previa after implementation of an autologous blood donation protocol. The authors reported that women who did not donate blood prepartum had a four times greater rate (12% versus 3.1%) of peripartum homologous blood transfusion. They recommended beginning blood donation at 32 weeks’ gestation with removal of 400 mL per week to achieve a total stored volume of 1,200 to 1,500 mL. Patients who donated autologous blood had a higher overall rate of blood transfusion, with 71% receiving blood peripartum compared with 12% of patients who received homologous blood. Although autologous blood has a slightly smaller risk of bacterial contamination, the risk of ABO mismatching is similar for both autologous and homologous blood. Consequently, the indications for transfusion of autologous blood are the same as banked blood.
6. Intraoperative cell salvage
Another alternative to homologous-banked blood is the use of an intraoperative cell salvage device, or cell saver. This technique involves suctioning of blood from the operative field followed by cell washing, suspension in saline, and reinfusion to the patient. Concerns about its possible association with amniotic fluid embolism (AFE) have made this technique controversial in the past but now it is used in most major centers.42
The cause of the coagulopathy and cardiovascular collapse associated with AFE is unclear. Contaminants including tissue factor, fetal squamous cells, meconium, and other particulates are present in amniotic fluid and may play a role in the development of AFE.43 Waters and colleagues44 demonstrated that when cells are washed and a leukocyte depletion filter is used, the resulting blood has a concentration of fetal squamous cells similar to a preoperative maternal blood sample. Another potential concern is that fetal hemoglobin is present in the processed cell saver blood, raising concerns about maternal alloimmunization and the potential for problems with subsequent pregnancies. Rh mismatch is particularly important and anti-D immune globulin should be administered to Rh-negative mothers who receive salvaged blood.
Cell salvage has been used safely in many patients and should be considered in patients at high risk for hemorrhage who would be difficult to cross match, object to blood transfusion (e.g., a Jehovah’s Witness with a known placenta accreta), or as a lifesaving measure. However, equipment and skilled personnel must be available.
7. Acute normovolemic hemodilution
Acute normovolemic hemodilution is a technique involving collection of autologous blood immediately prior to surgery or delivery. Normovolemia is maintained by IV fluid administration with colloid or crystalloid. The volume of colloid administered should be equal to the volume of blood withdrawn. When crystalloid is administered, the volume should be three times the volume of blood removed. When blood is subsequently lost, it has less red blood cell mass and the blood removed can be returned to the patient as needed.
Because the blood is collected and stored at the bedside for immediate reinfusion, the risks of bacterial contamination and administrative error associated with autologous blood storage are significantly reduced. This technique has been successfully reported in patients at risk for blood loss during CD, with an average of 1,000 mL of blood collected just prior to the surgery.45 In this study, no patients experienced symptoms of nausea, vomiting, dizziness, or light-headedness, and there were no abnormalities in vital signs or FHR.
8. Complications
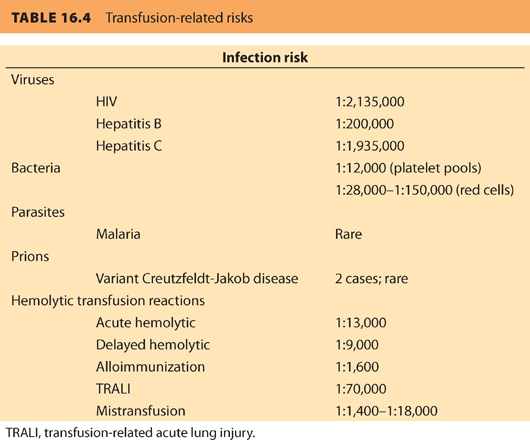
The risks of blood transfusion are summarized in Table 16.4.
9. Massive blood loss and transfusion
a. Definition
Massive transfusion is defined by administration of greater than 10 units of PRBCs. When massive blood loss occurs in obstetric patients, it is important to notify the blood bank. Communication between personnel, especially the obstetrician, anesthesiologist, and nursing staff regarding continued blood loss and the ongoing need for blood products, is important. A “code-white” or massive hemorrhage protocol is particularly helpful to outline responsibilities of nursing staff and personnel who are transporting blood products to the labor and delivery suite.46 Despite a recommendation for implementation of PPH protocols in every labor and delivery unit in the United States from the National Partnership for Maternal Safety,47 at least 20% of United States academic obstetric anesthesia units are without PPH protocols.48
b. Monitoring
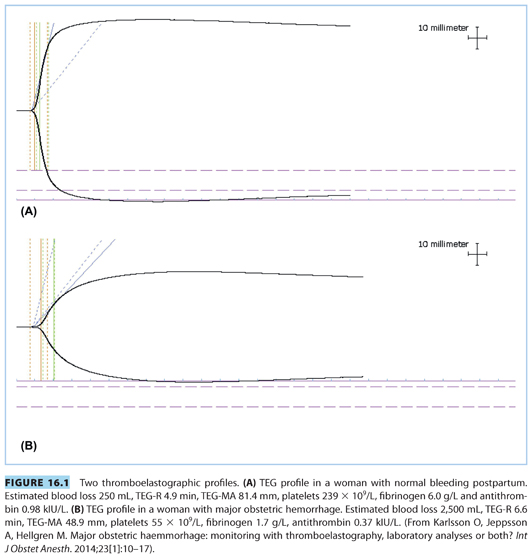
Adequate fluid resuscitation, appropriate monitoring, and therapy guided by laboratory tests are of prime importance in the management of obstetric hemorrhage. During massive blood loss, the patient must be reassessed frequently to evaluate effectiveness of treatment as well as to monitor for potential complications. At a minimum, two large cannulae (size 14 to 16 gauge) should be inserted. Fluid should be warmed to prevent hypothermia and this typically requires a blood infusion device with adequate warming capacity at high infusion rates. The goal of initial fluid resuscitation is to return the BP to low normal to ensure adequate tissue perfusion. The urine output and central venous pressure (CVP) are used to determine the adequacy of circulating volume. Urine output should be maintained at least at 0.5 mL/kg/hour and the CVP at 4 to 8 cm H2O. The anesthesiologist should keep in mind that CVP reflects right atrial filling pressure but is an inaccurate indicator of the left heart filling when the patient has cardiac or pulmonary disease. Thromboelastography (TEG) or rotational thromboelastometry (ROTEM) provide faster results than standard laboratory testing, which is advantageous in the setting of ongoing obstetric hemorrhage. Figure 16.1 presents an illustration of expected TEG tracings in obstetric coagulopathy. However, laboratory analyses (platelet count, activated partial thromboplastin time, prothrombin time, fibrinogen, antithrombin, and D-dimer) show greater differences in coagulation variables and may correlate better with estimated blood loss.49
c. Electrolyte balance
Electrolyte imbalance is common in hemorrhagic shock and requires attention. Hypokalemia is not unusual and is probably the consequence of a dramatic increase in catecholamine release during shock. This causes potassium to be transported into cells and is a temporary change that will self-correct if perfusion is restored. Treatment is generally not required unless the serum potassium concentration is <2.5 mEq per L or cardiac dysrhythmias are present. Hypocalcemia is often observed in patients who receive multiple blood product transfusions because the citrate anticoagulant chelates calcium. In addition, shock can result in failure of cellular ion pumps that export calcium from cells. The high intracellular calcium levels disrupt adenosine triphosphate (ATP) synthesis and myocardial contractility. Treatment should be considered if the ionized calcium level falls below approximately 1.5 mEq per L or if Q-T prolongation is seen on the electrocardiogram (ECG). Similarly, if hypomagnesemia occurs, replacement should be considered.
d. Dilutional coagulopathy
Patients with massive hemorrhage (greater than one blood volume) usually develop a dilutional coagulopathy from factor deficiency after IV crystalloid and/or colloid resuscitation. Fibrinogen levels decrease initially; the critical level of 1.0 g per L is likely to be reached after 150% blood volume loss, followed by a decrease of other labile coagulation factors to 25% activity after a 200% blood loss. Prolongation of the activated partial thromboplastin time (aPTT) and prothrombin time (PT) to 1·5 times the mean normal value is correlated with increased risk of clinical coagulopathy. Infusion of fresh frozen plasma (FFP) should be considered after blood volume is lost. The dose should be large enough to maintain coagulation factors well above the critical level. Experts advise that the platelet count should not be allowed to fall below the critical level of 50 to 100 × 109 per L in an acutely bleeding patient.
Treatment of dilutional coagulopathy is challenging and the primary monitoring tools are measurement of PT, aPTT, platelet count, and fibrinogen. Dilutional coagulopathy can also be detected by the use of thromboelastographic measurements (decreased maximum amplitude and/or α angle) and its use in obstetrics has been described.50,51 Calcium binding by the citrate preservative of blood products can become clinically significant in massive transfusion, leading to cardiac depression and hypotension. Patients often require calcium replacement to restore normal plasma levels. Studies of women with PPH have reported lower mean plasma fibrinogen levels (≤2 g per L) in women who go on to develop more severe PPH.52 The low fibrinogen concentrations in FFP limit its utility as a source of fibrinogen in transfusion.53 Cryoprecipitate has higher concentrations of fibrinogen54 but does not undergo viral inactivation procedures and carries the potential risk of patient exposure to blood-borne pathogens.55 In treating dilutional coagulopathy, the goal is for the platelet count to be higher than 50 × 109 per L and fibrinogen level >2 g per L.
e. Disseminated intravascular coagulation
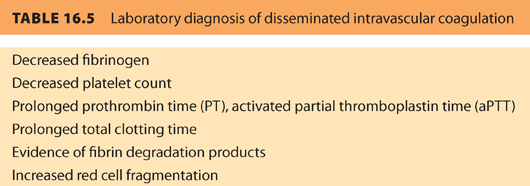
Disseminated intravascular coagulation (DIC) results from an underlying disease process (e.g., placental abruption, dead fetus syndrome, AFE, gram-negative sepsis, eclampsia, and retained products of conception) that initiates biodegradation of fibrinogen and clotting factors. This results in hemorrhage as well as microvascular thrombosis. Laboratory findings of DIC are listed in Table 16.5. Management includes treatment of the underlying disease with ongoing administration of blood products (i.e., PRBCs, platelets, clotting factors).

f. Activated recombinant factor VII
In life-threatening PPH, recombinant activated factor VII (rFVIIa) may be used as an adjunct to other surgical treatments, but there are no data to support the optimal timing of its use or recommended dose. A commonly used dose is 90 μg per kg, repeated once if no clinical response within 15 to 30 minutes. Adequate levels of platelet and fibrinogen are essential for rFVIIa to be effective,56 and these variables should be checked and corrected before administration of rFVIIa. This drug is also less effective in the presence of hypothermia and acidosis. The rFVIIa was originally developed to prevent or control bleeding in patients with hemophilia A or B with inhibitors to factors VIII or IX, but several reports have suggested decreased blood product requirements in surgical and trauma patients receiving rFVIIa during uncontrolled hemorrhage.
The rFVIIa augments the intrinsic clotting pathway by binding with tissue factor and directly activating factors IX and X. The dose is 50 to 100 µg per kg IV every 2 hours until there is evidence of hemostasis. Most patients require only one dose, but it is important to ensure adequate levels of platelets and other clotting factors because rFVIIa increases clotting by acting on these substrates. The optimal timing for administration has not been described, but rFVIIa should only be considered in life-threatening obstetric hemorrhage when other management strategies have failed. Most complications resulting from rFVIIa are associated with thrombosis, myocardial infarction, pulmonary embolism, and clotting of vascular access devices.
g. Tranexamic acid is an antifibrinolytic agent. Investigations have been conducted to determine if it is useful for both prevention and treatment of PPH because its hypothesized mechanism of action is to supplement uterotonics and because it has been proved to reduce blood loss in elective surgery and bleeding in trauma patients. Although results are promising in the treatment of PPH after vaginal delivery or CD, large multicentre randomized controlled trials will be required before widespread use can be recommended.57
B. Antepartum hemorrhage
Antepartum hemorrhage complicates nearly 10% of all pregnancies. Although most of these cases are not serious and result from minor complications (e.g., cervicitis), others result from abnormal placentation (e.g., placenta previa, placental abruption). These more serious causes of hemorrhage are a threat to fetal and maternal well-being.
Obstetricians ask the following questions when evaluating patients with antepartum hemorrhage:
• Does the bleeding threaten the life of mother and/or fetus?
• What is the cause of hemorrhage?
• When and how should the fetus be delivered?
1. Placenta previa
a. Definition
The placenta normally implants in the upper uterine segment. In placenta previa, the placenta either totally or partially implants over or very near the internal os. Because it presents before the fetal presenting part, it obstructs fetal descent. This condition affects approximately 0.5% of pregnancies.
b. Epidemiology
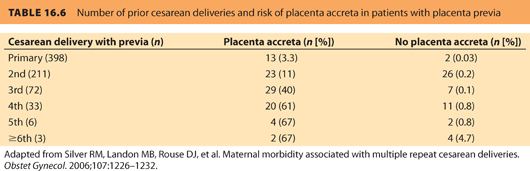
Placenta previa complicates 4.8 per 1,000 deliveries annually and is fatal in approximately 0.03% of cases. The exact cause is uncertain, but prior uterine surgery is a common factor in most cases. Risk factors include (1) advanced maternal age, (2) multiparity, (3) smoking history, (4) prior CD or other uterine surgery (e.g., myomectomy), and (5) previous placenta previa. Women with placenta previa are at an increased risk for abruptio placentae (relative risk [RR], 13.8), CD (RR, 3.9), fetal malpresentation (RR, 2.8), and PPH (RR, 1.7).58 Women with placenta previa and a prior history of CD are also at increased risk for placenta accreta59 (see Table 16.6).

Full access? Get Clinical Tree







