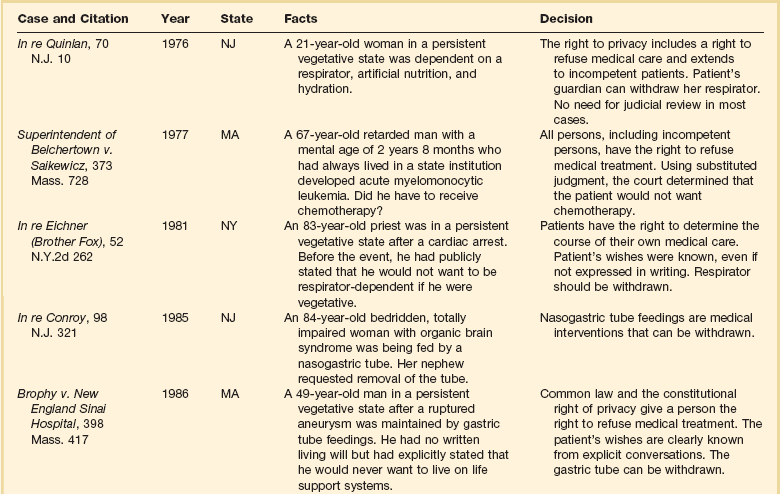
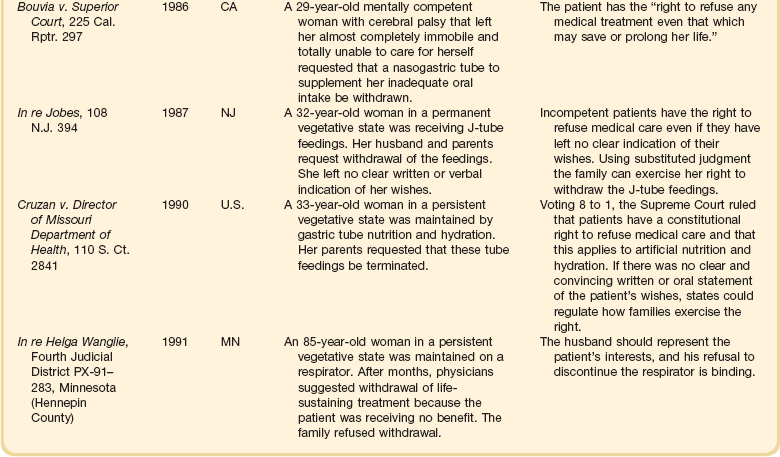
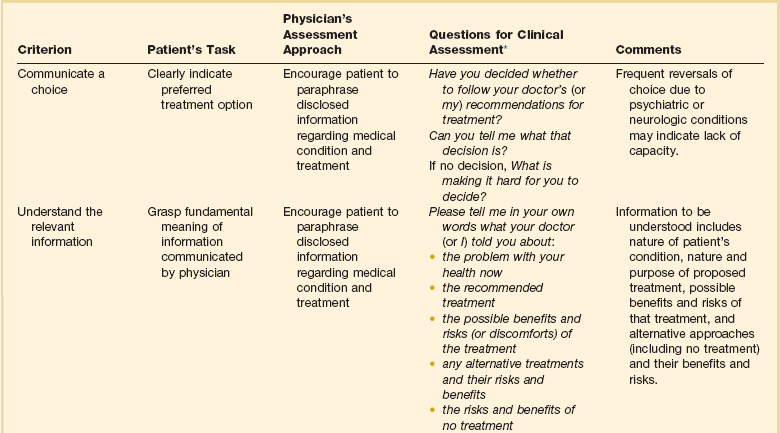
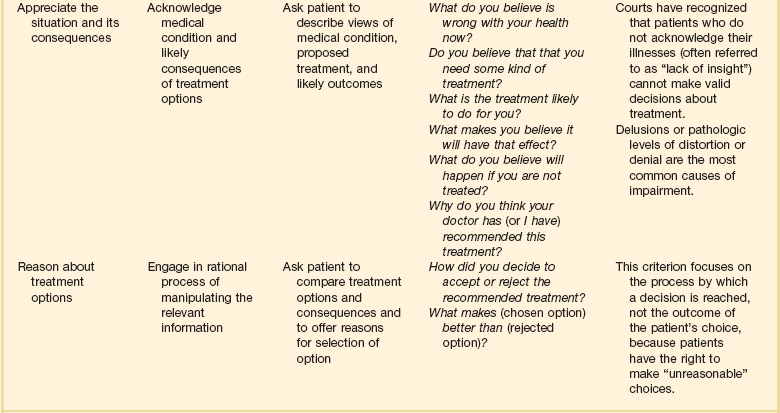
71 THE DOCTOR-PATIENT RELATIONSHIP Decision Making for Cognitively Impaired Patients Avoiding Conflicts in the Intensive Care Unit Disparity in Use and Outcome of Intensive Care THE ETHICS OF END-OF-LIFE CARE Withholding and Withdrawing Life-Sustaining Treatments Advance Care Directives and Durable Powers of Attorney Ethical Issues in Transitioning Patients to Palliative Care RESEARCH IN CRITICALLY ILL PATIENTS History and Fundamentals of Human Research Ethics Putting Principles into Practice: Applications Research in the International Context Collection and Storage of Tissue Samples for Future Unspecified Research, Particularly Genetic Research Critical illnesses and the interventions necessary to address them pose many ethical dilemmas for clinicians. Therefore, it is not surprising that critical care physicians encounter ethical dilemmas more often than do general internists.1 The most frequent predicaments relate to end-of-life care, including decisions about termination of medical treatment, respect for patient autonomy, and conflicts among various parties involved in patient care. Less frequent quandaries stem from concerns about equitable use of resources, truth telling, religious and cultural differences, and professional conduct. On rare occasions, critical care providers must be prepared to address the extraordinary demands related to disasters because the skills and resources at their command offer key components of a well-organized disaster response. As a rule, clinicians should follow the same ethical guidance in critical care situations as in less stressful contexts:2 They should treat patients with respect. They should deal honestly with patients and should not reveal confidences entrusted to them, unless the well-being of others is threatened. They should act in good faith, keep promises and commitments, and try faithfully to meet fiduciary responsibilities to patients. At the same time, ICU staff must balance competing moral obligations that may limit or override obligations to fidelity to one particular patient, such as the needs of other patients who are currently under their care or may need their care in the future. Various models of decision making have been proposed—ranging from an informative model, in which patients make the decisions quite independently after the clinician has offered sufficient information, to a more paternalistic model, in which clinicians make decisions based on their judgment of what is in the best interest of the patient.3 A commonly accepted model today is a deliberative model, in which the clinician gives the patient information about his or her condition and the medical options, along with their advantages and disadvantages, and the patient explains his or her values and preferences, and together they reach a treatment decision. This model must be adapted to the extreme circumstance of critical illness.4,5 Leaders in the field of critical care medicine have endorsed a model of decision making, shared decision making, that recognizes that patients and their surrogates will vary in their desire to participate in decision making, but generally all will feel most comfortable with decisions if they have been given sufficient information to be able to understand and trust the decision process.6–9 Most physicians do not follow the same model with every patient or in every encounter. Regardless of the model adopted, clinicians should heed the elements of good ethical practice when making their decisions (Box 71.1). ICU clinicians also should be attentive to the many facets of patients’ lives that influence their views and preferences. For example, patients’ families play a large role in shaping their experiences and beliefs and in supporting them, particularly when they are sick. Ethicists in North America initially took an approach to patient autonomy that ignored the family, but more recent thought has recognized the importance of the family’s supportive role.10,11 Clinicians also should be sensitive to the needs of the family when a patient is sick.12 Among these, according to a survey of family members in ICU waiting rooms, are the need to talk about negative feelings such as guilt and anger; to talk about the possibility of the patient’s death; to be told what to expect before they go into the ICU for the first time; to visit at any time; to talk to the same nurse every day; to receive explanations that are understandable; to feel that there is hope; to have good food available in the hospital; to be assured that it is all right to leave the hospital for a while; and to feel accepted by the staff.13 Members of the ICU staff also should take note of the religious affiliation and cultural identity of their patients. However, they should not stereotype patients and presume to know what patients want based on their affiliation, but rather should be ready to inquire about each patient’s views and should be respectful of diverse beliefs14,15 (Box 71.2). Often, the ICU clinician must convey bad news. Recommendations for breaking bad news include the following16: • Use a location that is comfortable, quiet, and private. • Set aside adequate time for discussion. • Check what the patient or family already knows. • Give some warning that there will be unfortunate news. • Let the patient’s desire for information guide the discussion. • Elicit and address the patient’s reactions and concerns. • Foster an appropriate level of hope. Communication with ventilated patients is particularly difficult. Clinicians should make every effort to use techniques designed to overcome communication barriers with ventilated patients.17 Because many patients are, or may become, cognitively impaired, clinicians should frequently and repeatedly assess patients’ capacity to understand their situation and make decisions. Judging the capacity of patients to make decisions can be difficult.18,19 Table 71.1 shows recommendations for assessing the relevant criteria: the ability to communicate a choice, to understand the relevant information, to appreciate the situation and its consequences, and to reason about treatment options. When patients are capable of decision making, they should be involved to the extent that they desire. Patients who have not prepared advance directives should be asked if they would like to prepare such a directive and should be asked to designate someone to hold durable power of attorney for them. Table 71.1 Legally Relevant Criteria for Decision-Making Capacity and Approaches to Assessment of the Patient *Responses need not be verbal. From Appelbaum PS: Assessment of patients’ competence to consent to treatment. N Engl J Med 2007;357:1834-1840. Care in the ICU is provided by a multidisciplinary team; good collaboration among its members is essential. Paying attention to the perspectives of all team members and respecting their skills and clinical judgment are ethically important and are associated with improved clinical outcomes.20 Collaboration is valuable not only for individual patients’ care but also to achieve optimal function of the unit as a whole.21 Of interest, Baker and Strosberg have argued that the assumption that triage is based on a utilitarian theory of justice is not correct.22 They point out that triage was developed by Larrey, surgeon general of Napoleon’s army, as a strategy for systematically handling the wounded so that those who had to be attended to first got care without regard to rank, in keeping with the French Revolutionary commitment to liberty, equality, and fraternity. Baker and Strosberg suggest that an egalitarian form of triage is advantageous because the public is likely to voluntarily comply with it. Persons with normal “rational self-interest” would agree with it because it improves everyone’s chances of survival. The chances of survival of the fatally wounded and the slightly wounded would not be significantly altered by deferred treatment. This optimal arrangement thus also is compatible with a social contract theory of justice.23 Although triage strategies have relied on the probability of survival, some authors have argued that this is too crude an outcome measure to guide triage. Engelhardt and Rie have suggested that critical decisions to admit, continue care, or discharge patients should be based on a more complete formula that includes probability of successful outcome, quality of life, predicted length of life remaining, and cost of therapy.24 The Task Force on Guidelines of the Society of Critical Care Medicine (SCCM) and the American College of Critical Care Medicine (ACCM) have published recommendations for ICU admission and discharge.25,26 Each ICU should create a specific policy that explicitly articulates admission and discharge criteria and defines the services that it provides to the population served. Compliance with the policy should be monitored, and the policy should be revised as needed. Any decision to deny a patient admission should be made by clinicians who are familiar with expert opinion and relevant literature and should use established guidelines. Standardized criteria and guidelines facilitate fair rationing because they enhance the likelihood that patients will be treated similarly. Discharge decisions should be guided by an assessment that less care is necessary and should take patient safety into account. Decisions to transfer a patient from the ICU to other hospital facilities should always be accompanied by good communication with the receiving team to avoid oversights and errors in care.27 Straightforward indications would include, at one extreme, improvement in medical condition that obviates the need for further intensive therapy or, at the other extreme, a decision to end intensive care because of impending death. The ethically challenging aspect of discharge criteria involves the question of discharge when a patient’s probability of survival is expected to be only minimally improved by remaining in the ICU, but the probability is not zero. Triage decisions should be made explicitly and without bias. Ethnicity, race, gender, social status, sexual preference, and financial status should not be considered.26 Factors that are appropriate to consider include probability of survival; likely functional outcome; age; chronic underlying conditions; marginal benefit to be gained; and preferences expressed by the patient or surrogate.28 When the ICU is full, patients already in the ICU should not necessarily be given priority if someone else stands to benefit more from the care.29 Like many ethically difficult decisions, triage decisions can be made more manageable by thinking proactively, every day, about the disposition of patients. For example, ICU physicians should regularly review the status of all patients in the unit to assess their degree of readiness for discharge in case the need for new admissions arises.27 Application of this kind of strategy should involve cooperation with other patient care units in the hospital to arrange smooth transfer. Even when policies are in place for fair triage through an admission approval process by a designated individual, attempts to circumvent admission rules by seeking permission from ICU clinicians or administrators who are on duty in the ICU are fairly common.30 Therefore, policies should be designed to anticipate—and resist—such backdoor efforts. In addition to decisions about admission, discharge, and triage, ICU physicians frequently must deal with the question of whether to offer or withhold treatments from patients with ultimately fatal injuries or illnesses. The ethical reasoning behind decisions to ration possibly beneficial interventions should be clear in the clinician’s mind31; this issue is discussed more fully later in the section on termination of medical care. Because expected benefit is a crucial factor in decision making, it is important for critical care physicians to understand the limits of prognostic guidelines for patients with life-threatening illnesses.32 Physicians should recognize the degree of uncertainty that surrounds mortality estimates. Although it is useful to consider a patient’s expected outcome, and to use this prognosis to guide decisions, a false sense of certainty can lead to mistakes. Furthermore, communicating prognostic information with a false sense of certainty can lead to misunderstanding and subsequent distrust on the part of families. Prognostic scoring systems can serve as a useful baseline on which to build treatment recommendations, but firm thresholds should not be set. For a patient with a very uncertain prognosis, trying different treatments for short periods can avoid extended inappropriate treatments without denying care that has a minute chance of working. Medical decision making requires more than functional assessment and prediction. Scoring systems can provide an unbiased measure to help inform physicians’ decisions, but such measures should not be adopted as absolute guides.32 Critical care clinicians should be aware that a number of studies show a pattern of disparity in use of intensive care that is the result of forces outside the ICU itself. Patients of lower socioeconomic status have higher mortality rates.33 Patients who lack health insurance are less likely to be admitted to hospitals; once hospitalized, however, they are more likely to be admitted to the ICU and more likely to die in the hospital.34 Patients with private attending physicians are likely to stay longer in the ICU. Intensive care providers should try to prevent inequitable use of resources in the delivery of critical care services. Given the emphasis on life and death decisions in intensive care, it is prudent for the critical care practitioners to be aware of the many philosophical questions surrounding the definition of death.36 In any consideration of the definition of death, it is useful to recognize that death is more of a process than an instantaneous event and that the boundary between life and death is not perfectly sharp. The specification of any standard will require some arbitrary line drawing that has ethical implications.36 In 1968, the Ad Hoc Committee of the Harvard Medical School to Examine the Definition of Brain Death determined that severely brain injured patients meeting certain diagnostic criteria could be declared dead prior to the cessation of cardiopulmonary function.37 The use of neurologic criteria to determine death was subsequently accepted by some states in the United States. However, confusion remained with regard to what constituted “brain death”; specifically whether total brain nonfunction or brainstem nonfunction sufficiently fulfilled neurologic criteria for death. In response to the variability in state statutes regarding brain death, the President’s Commission for the Study of Ethical Problems in Medicine published a uniform statute for determining brain death, called the Uniform Determination of Death Act (UDDA). According to the UDDA, “an individual who has sustained either 1) irreversible cessation of circulatory and respiratory function or 2) irreversible cessation of all functions of the entire brain, including the brainstem is dead. A determination of death must be made in accordance with accepted medical standards.”38 The ethical justification for using neurologic criteria to determine death relies on the presumption that in brain death, the body of the patient is no longer “a somatically integrated whole” and that in the absence of whole brain function, maintaining circulation, even with cardiorespiratory support, will stop imminently within a defined period of time.39 Recently the use of brain death criteria has been questioned in the medical and bioethical community. Opponents of using brain death criteria cite the uncertainty in determining physiologic death by neurologic parameters. There is evidence that even in the setting of whole brain death many homeostatic functions can persist, including maintenance of body temperature, wound healing, the gestation of a fetus in a pregnant patient, and sexual maturation and growth in pediatric patients who fulfill the neurologic criteria for death.40 In addition, cardiopulmonary death does not always occur in a timely fashion after brain death and in rare cases may take weeks or years to occur after brain death has been declared.41 Notably, arguments against neurologic standards of death do not preclude the ethical permissibility of withdrawing supportive care when the criteria of brain death have been met, but question whether these criteria alone constitute the death of the patient. In response to concerns regarding brain death as a legitimate determinant of human death, the President’s Council on Bioethics revisited the philosophical and clinical dilemmas surrounding this issue in 2008.39 The council’s ultimate conclusions were to support neurologic criteria of brain death with an alternative argument regarding defining death as the inability of the organism to function as “a somatically integrated whole.” Rather, “total brain failure” constitutes death as the patient, “is no longer able to carry out the fundamental work of a living organism. Such a patient has lost—and lost irreversibly—a fundamental openness to the surrounding environment as well as the capacity and drive to act on this environment on his or her own behalf . . . a living organism engages in self-sustaining, need-driven activities critical to and constitutive of its commerce with the surrounding world. These activities are authentic signs of active ongoing life. When these signs are absent, and these activities have ceased, then a judgment that the organism as a whole has died can be made with confidence.” Currently all 50 states and the District of Columbia have adopted the UDDA definition of brain death by statute or judicial decision. Two states, New Jersey and New York, have specific laws or regulations to address religious objections to neurologically based declarations of death.42 Similarly, over 90 countries use neurologic criteria to determine death in addition to traditional cardiopulmonary criteria.43 The cultural variability in accepting neurologic criteria to determine brain death is exemplified in the organ transplant laws in China and Japan. In 2003, the Chinese Ministry of Public Health drafted a proposal to outline neurologic criteria that would define death in the absence of cardiopulmonary arrest. However, legislation approving the use of brain death criteria was not endorsed, lacking support from the public and health care professionals.43 Prior to 2010, Japan’s Organ Transplant Law only recognized brain death when the patient had given prior written consent to be an organ donor and the family did not object to the donation. This law has since been revised to allow a determination of death based on neurologic criteria for the purposes of organ donation with family consent so long as the donor did not previously refuse organ donation. However, the revision still does not address whether neurologic criteria for death are sufficient in the absence of an anticipated organ donation.44 The first suggestion that physicians should withhold medical interventions from terminally ill patients probably dates to Hippocrates’s injunction to “refuse to treat those [patients] who are overmastered by their disease, realizing that in such cases medicine is powerless.”45 In 1835, Jacob Bigelow urged members of the Massachusetts Medical Society to withhold “therapies”—such as cathartics and emetics—from hopelessly ill patients.46 In 1848, John Warren, the surgeon who performed the first operation with ether anesthesia, urged that ether should be used “in mitigating the agonies of death.”47 In 1958, Pope Pius XII, in response to questions about resuscitating patients and maintaining comatose patients on respirators, stated that physicians had no obligation to use such “extraordinary” means to forestall death.48 The concept that the mere extension of life is not always in the best interest of the patient is perhaps even more apparent in current times, when advances in medical technology have led to the seemingly indefinite prolongation of the lives of the critically and terminally ill.49 Many physicians find withdrawing life-sustaining treatment more difficult than withholding treatment. However, from a bioethical perspective, there is little distinction between withholding and withdrawing life-sustaining treatments.50 Competent patients have the right to refuse medical care and can use whatever criteria they deem acceptable; it is their values that guide the choice.51 Every medical intervention, including artificial nutrition and hydration, may be terminated under some conditions. The right to refuse medical interventions, including life-sustaining treatment, is supported by legal precedent (Table 71.2). Court decisions have sanctioned the withholding or withdrawal of respirators, chemotherapy, blood transfusions, hemodialysis, and major surgical operations. In its 1990 Cruzan decision, the U.S. Supreme Court recognized that competent patients have a constitutional right to refuse medical care.52 Competent patients need not be terminally ill to exercise the right to refuse interventions; they have the right regardless of health status. Moreover, the right applies both to withholding proposed treatments and to discontinuing initiated treatments. This does not, however, imply that patients have a correlative right to demand treatment.53,54 In theory, the right of patients to refuse medical therapy can be limited by state interests in the preservation of life, prevention of suicide, protection of third parties such as children, and preservation of the integrity of the medical profession.54 In practice, these interests almost never override the rights of competent patients or of incapacitated patients who have left explicit advance directives. There are two types of advance care planning documents: living wills and proxy statements. Living wills or instructional directives are advisory documents specifying the patient’s preferences to specific care decisions. State-specific forms that people can fill in to draw up advance directives are available on the Internet.55 Some advance directives, such as the Medical Directive, enumerate different scenarios and interventions for the patient to choose from.56 Among these, some are for general use and others are designed for use by patients with a specific disease, such as cancer.57 Less specific directives can be general statements of not wanting life-sustaining interventions or forms that describe the values that should guide specific terminal care decisions. Of importance, a person does not have to use a state-specific form because “a living will or health care power of attorney that does not strictly follow the statutory [state] form is also valid in most states” and the U.S. Supreme Court has ruled that a person has a constitutional right to refuse medical treatments.58 Practitioners should be aware that living wills may have some legal limitations. For instance, in 25 states, a living will is not valid if a woman is pregnant; specific state statutes should be reviewed in caring for a pregnant patient. The health care proxy statement, sometimes called a durable power of attorney for health care, specifies a person selected by the patient to make decisions. A combined directive includes both instructions and the designation of a proxy; the directive should clearly indicate whether the specified patient preferences or the proxy’s choice should take precedence if they conflict.56 Many states permit clear and explicit verbal statements to be legally binding even if not written down.58 However, such statements must be very explicit. In the Wendland case, a 42-year-old man suffered permanent brain damage and hemiparesis in a car accident.59 The California Supreme Court ruled that when the patient is conscious and there is no advance care directive, there must be “clear and convincing” evidence of the patient’s view in order to permit withdrawal of a feeding tube.59 “Clear and convincing” evidence requires prior comments to refer to the specific intervention in the specific circumstances of the patient, not a similar health state. In 1984, California passed the first law recognizing the appointment of a designated proxy for health care decisions; by 2007, all 50 states and the District of Columbia had enacted statutes recognizing the durable power of attorney for health care decisions. There are some limitations. For instance, although most states permit proxies to terminate life-sustaining treatments, Alaska prohibits such decisions by proxies. In other states, orally appointed proxies are limited to a particular hospitalization or episode of illness. Nevertheless, it appears that any properly filled-out, formal advance care document or durable power of attorney designation, whether or not it conforms to a state’s specific document, is protected by the U.S. Constitution and must be honored.52 Although advance directives can be helpful in guiding clinicians and family members, many patients have not prepared them. Despite polling data showing that approximately 80% of Americans endorse the use of advance directives, and passage in 1990 of the federal Patient Self-Determination Act (PSDA), which requires hospitals and other health care facilities to inform patients about their right to complete an advance care directive, less than 30% of the adult population in the United States has a formally prepared advance directive.60 The use of advance care directives may be more prevalent in older adults. Silveira and colleagues used data from the Health and Retirement Study to survey the proxies of patients 60 years and older who had died between 2000 and 2006 and found that approximately 47% of these patients had advance directives.61 However, even when advance care directives have been prepared, they frequently are not in the patient’s medical record, and the patient’s physician may not be aware of the existence or content of the document.62,63 In addition, recent studies suggest that most advance directives are either proxy forms or standard living wills, and that few have any specific directions from the patient.64 Finally, studies confirm that proxies and family members tend to be poorly informed about patients’ wishes regarding end-of-life care and therefore are unlikely to make decisions as the patient would.65,66 Even if specific treatment courses are outlined, these directives may be outdated as preferences change with time or the patient’s medical condition evolves. Ideally, advance directives should be revisited with the patient over time with family members or a physician with whom the patient has a long-term relationship. In the late 1980s and early 1990s, some argued that physicians could ethically terminate futile treatments.67 However, citing medial futility as an ethical and legal justification for the withdrawal of life-sustaining treatments is not a clear-cut endeavor and has been criticized as inadvisable.68,69 The term futility carries both quantitative and qualitative meanings. There is little, if any, agreement among health care professionals as to what numeric threshold of probability should be considered an indication of futility. Medical futility also has a qualitative aspect that implies that the objective of the proposed treatment is not worthwhile.42 The qualitative definition of futility can be especially problematic when patients or their surrogate decision makers disagree with physicians about what constitutes a worthwhile outcome. In addition, a declaration by clinicians that a treatment is futile can marginalize patients and surrogates by effectively revoking their participation in treatment decisions. Thus, the ambiguities in defining medical futility and the potential for alienation of patients and family members have led some bioethicists to propose that the term futility be replaced by the terms “medically inappropriate” or “surgically inappropriate” to more accurately describe an assessment that reflects a professional opinion rather than a summation of value.70 Nonetheless, some states including Texas, Virginia, Maryland, and California have enacted so-called medical futility laws.71 These laws protect physicians from liability if they terminate life-sustaining treatments against family wishes. In Texas, if the medical team and the hospital ethics committee believe that interventions should be terminated, but the patient’s family disagrees, the hospital is supposed to seek another institution willing to provide treatment.71 If, after 10 days, this fails, then the hospital and the physician may unilaterally withdraw treatments determined to be futile; however, the family may appeal to a state court. Early data suggest that the law increases futility consultations with the ethics committee, and that most families concur with withdrawal decision.71 Some hospitals have enacted “unilateral DNR” (do not resuscitate) policies to allow clinicians to provide a DNR order in cases in which consensus cannot be reached with families and there is medical opinion that resuscitation would not affect a patient’s outcome. Because the ethical justification for unilateral DNR relies on the medical assessment that resuscitation efforts will not achieve the desired outcome (i.e., resuscitation is futile) the unilateral DNR remains a controversial policy. If a unilateral DNR is being considered by a physician, a second opinion by another physician and a hospital ethics committee consultation should be considered.42 “Partial codes” and “slow codes” describe resuscitation efforts that are selective or foreshortened in the setting in which the medical team believes resuscitation efforts to be inappropriate and the patient’s family or proxy will not agree to a recommended DNR order. Slow codes have been historically almost universally repudiated in the bioethics community. The American College of Physicians Ethics Manual cautions against slow codes as “deceptive, half-hearted resuscitation efforts.”72 Ultimately slow and partial codes threaten the ethical principles of autonomy and beneficence. By neither attempting a full resuscitation nor invoking a unilateral DNR, the patient’s or surrogate’s decision is disregarded while administering a nonbeneficial treatment. However, more recently Lantos and Meadow have defended the practice of partial and slow codes when communication has been exhausted and intractable disagreements about cardiopulmonary resuscitation (CPR) persist.73–75 Supporters of the slow or partial code cite the symbolic value of CPR and delineate specific circumstances in which such a limited code would be ethically permissible such as when resuscitation will almost certainly be ineffective, the surrogate decision makers understand that death is inevitable, and the surrogates “cannot bring themselves to agree to a do-not-resuscitate order.”73 When compared to enforcing a unilateral DNR on a surrogate or family member, such a compromise may be a more compassionate option for those responsible for making a decision on DNR status. However, arguments supporting limited resuscitation are almost always focused exclusively on the welfare of the surrogates, rather than the patient under the physician’s care. Therefore, slow and partial codes should not be considered an acceptable practice in the care of critically ill patients. Following Pope Pius XII’s and Roman Catholic teachings, some ethicists advocate a distinction between ordinary and extraordinary care: Ordinary care is considered to be mandatory, whereas extraordinary care may be withheld or withdrawn.48 One commentator for the Catholic Hospital Association explained this distinction as follows: Ordinary means of preserving life are all medicines, treatments, and operations, which offer a reasonable hope of benefit for the patient and which can be obtained and used without excessive expense, pain, or inconvenience. . . . Extraordinary means of preserving life mean all medicines, treatments, and operations, which cannot be obtained without excessive expense, pain, or other inconvenience, or which, if used, would not offer reasonable hope of benefit.76 Many ethicists and courts have concluded that this distinction is too vague and has “too many conflicting meanings” to be helpful in guiding surrogate decision makers and physicians.53,54,77,78 As one lawyer noted, ordinary and extraordinary are “extremely fact-sensitive, relative terms. . . . What is ordinary for one patient under particular circumstances may be extraordinary for the same patient under different circumstances, or for a different patient under the same circumstances.”78 Thus, the ordinary versus extraordinary distinction should not be used to justify decisions about stopping treatment.54 The standard of substituted judgment is based on preserving the patient’s right of self-determination in the absence of decisional capacity. Many courts advocate use of the substituted judgment criterion. Substituted judgment holds that the surrogate decision maker should try to imagine what the patient would do if the patient were competent.77
Ethical Considerations in Managing Critically Ill Patients
The Doctor-Patient Relationship
Communication with Patients
Decision Making for Cognitively Impaired Patients
Collaborative Care
Justice-Related Issues
Admission Criteria
Discharge Criteria
Triage
Disparity in Use and Outcome of Intensive Care
The Ethics of End-of-Life Care
Defining Death
Withholding and Withdrawing Life-Sustaining Treatment
Advance Care Directives and Durable Powers of Attorney
Futile Treatments
Ordinary/Extraordinary Care
Substituted Judgment

Full access? Get Clinical Tree


Ethical Considerations in Managing Critically Ill Patients