CHAPTER 21 Congenital Cardiac Anesthesia: Non-Bypass Procedures
The population of children and adults who has undergone successful repair or palliation of congenital heart disease (CHD) continues to increase (Warnes and Deanfield, 2001; Warnes et al., 2001). Approximately 85% of infants born with CHD can expect to reach adulthood (Moller et al., 1994), and because children of parents with CHD have an increased incidence of CHD (Hoffman et al., 2004), the total incidence and prevalence of CHD are likely to increase generation by generation. Although CHD is synonymous with childhood, the number of adults with CHD currently equals, and is predicted to exceed, the number of children with CHD (Webb and Williams, 2001); the total number in the United States alone may be approaching 500,000 individuals with significant versions of palliated CHD. The heterogeneous nature of the CHD population is made more so by the use of different treatment strategies for the same or similar lesions, in conjunction with advances in pediatric cardiac surgery, interventional catheterization, and electrophysiologic techniques. For example, in transposition of the great arteries (D-TGA), the majority of adults have had the atrial switch operation (the Mustard or Senning procedure), whereas most children have had the arterial switch operation (the Jatene). These two operations for the same underlying condition carry vastly different intermediate and long-term outcomes (Williams and Webb, 2000; Warnes, 2006).
Although it is common to differentiate between corrective and palliative surgery, total correction or cure is not the rule for the majority of children with CHD (Stark, 1989). Cure or definitive repair, in the strictest sense, means that normal cardiovascular structure and function are achieved and maintained; life expectancy is normal; further medical, surgical, and catheter-based treatments for the CHD are unnecessary; and noncardiovascular (e.g., renal, neurologic) consequences are nonexistent. With cure, there are no cardiac or vascular residua (abnormalities that were part of the original defect and are still present after repair), sequelae (disorders intentionally incurred at the time of reparative surgery and deemed unavoidable), or complications (unintentional aftermath) after surgery (Perloff, 1997). Palliative repair implies that future procedures are anticipated or necessary to maintain or restore the patient to a state of normal (or at least compensated) physiology and to improve life span. Lesions that lend themselves to cure are uncomplicated closure at an early age of an uncomplicated, nonpulmonary hypertensive patent ductus arteriosus (PDA), atrial septal defect (ASD), ventricular septal defect (VSD) (Talner et al., 1980), and in some instances catheter ablation of tachyarrhythmias (Walsh, 2007). Virtually all other forms of CHD require long-term surveillance. Many carry substantial risk for residual and potentially progressive structural, contractile, hemodynamic, electrophysiologic, and end-organ abnormalities.
Cardiac factors influencing outcome and anesthetic risk
The factors that determine the natural history and pathophysiologic consequences of congenital cardiovascular malformations also affect perioperative risk. Although the majority of anesthesiologists are not familiar with the natural history of each and every lesion, it is possible to develop a rational approach to the anesthetic management of this group of patients by focusing on the factors listed in Box 21-1. Identification of patients at increased risk, and development of an appropriate strategy to prevent adverse events is the cornerstone of anesthetic management.
Shunting
A shunt is an abnormal communication between the systemic and pulmonary circulations, allowing blood to flow directly from one circulatory system to the other. A left-to-right shunt allows oxygenated pulmonary venous blood to return directly to the lungs rather than being pumped to the body, whereas a right-to-left shunt allows deoxygenated systemic venous blood to bypass the lungs and return to the body (Sommer et al., 2008). An increased workload is placed on the ventricles, with the degree (volume) of shunting determining the severity of symptoms. Factors influencing the direction and degree of shunting include the size of the shunt orifice, the pressure gradient between the chambers or arteries involved in the shunt, the relative compliance of the right and left ventricles, the ratio of pulmonary vascular resistance (PVR) to systemic vascular resistance (SVR), and the blood viscosity (hematocrit). Total pulmonary blood flow (QP) is the sum of effective pulmonary blood flow and recirculated pulmonary blood flow, whereas total systemic blood flow (QS) is the sum of effective systemic blood flow and recirculated systemic blood flow. Total QP and total QS do not have to be equal.
The lesions most likely to be encountered before repair that are associated with the potential for left-to-right shunting include large PDA, VSD, and atrioventricular canal defects; patients palliated with large, unobstructed modified Blalock-Taussig shunts (e.g., stage I repair of hypoplastic left heart syndrome) can behave similarly. Left-to-right shunting results in increased pulmonary blood flow, increased pulmonary vascular resistance, increased pulmonary artery pressures (PAP), increased left atrial volume or pressure, pulmonary edema, and volume overload of both the right and left ventricles leading to biventricular failure. Low aortic diastolic pressure accompanying large systemic-to-pulmonary artery shunts can lead to myocardial ischemia as well as organ hypoperfusion (e.g., bowel ischemia). Pulmonary overcirculation is associated with decreased lung compliance, increased airway resistance (Stayer et al., 2004), and airway compression (Berlinger et al., 1983). Alterations in pulmonary function lead to increased work of breathing (with increased energy expenditure), atelectasis, air trapping, and respiratory infections. The time course for developing pulmonary vascular occlusive disease (PVOD) with shunt reversal (right-to-left) and Eisenmenger’s syndrome depends on the size and site of the shunt and age at repair; patients with underlying anatomic or genetic predisposition to the development of pulmonary hypertension—for example, trisomy 21 children—can develop earlier, more severe PVOD for a given shunt (Chi and Krovetz, 1975; Gorenflo et al., 2002).
Right-to-left shunting results in decreased oxygen content of the systemic arterial blood, with the decrease in proportion to the volume of deoxygenated systemic venous blood mixing with the oxygenated pulmonary venous blood. Even with normal cardiac output, the decrease in tissue oxygen delivery limits exercise tolerance (Sommer et al., 2008).
Ventricular Dysfunction
Progressive ventricular dysfunction leading to congestive heart failure (CHF) is the most common cause of disability and death in patients with CHD (Warnes and Deanfield, 2001). The etiology is multifactorial and may result from the primary disease, many years of abnormal volume and pressure loading (which cause pathologic remodeling of numerous cardiomyocyte and nonmyocyte functions and processes), chronic hypoxemia, damage during surgical repair (inadequate myocardial preservation, scarring, poor repair, damage to coronary arteries), acquired disease (Graham, 1982), and arrhythmias (Shinbane et al., 1997; Deal, 2001). Ventricular volume overload occurs with intracardiac or extracardiac left-to-right shunts, valvular regurgitation, and single-ventricle lesions. The time course over which irreversible ventricular dysfunction develops is variable, but if surgical intervention to correct the volume overload is undertaken within the first year of life, residual dysfunction is uncommon (Cordell et al., 1976; Graham et al., 1976). Ventricular pressure overload results from residual or recurrent ventricular outflow obstruction or elevated PAP or PVR. The time to develop significant ventricular dysfunction is longer compared with a chronic volume load, so symptoms are uncommon unless the obstruction is severe and prolonged, or it is combined with a volume load (Graham, 1991). Chronic hypoxemia and cyanosis decrease ventricular oxygen supply and increase oxygen demand through increased work related to increases in pulmonary and systemic vascular resistance with associated polycythemia. Myocardial ischemia resulting from coronary artery anomalies or kinking or torsion after reimplantation may also cause ventricular dysfunction.
Ventricular Outflow Obstruction
Ventricular outflow obstruction may be subvalvar, valvar, supravalvar, or a combination thereof, isolated or part of more complex malformations, residual or recurrent, and fixed or dynamic. Outflow obstruction results in pressure overload on the ventricle, ventricular hypertrophy, a “stiff” ventricle (diastolic dysfunction), and ultimately systolic ventricular dysfunction (Carabello, 2006). Left ventricular outflow obstruction may occur with aortic stenosis, coarctation of the aorta, interrupted aortic arch, and variants of HLHS and Shone’s anomaly (Shone et al., 1963). Right ventricular outflow obstruction is seen with pulmonary stenosis, TOF, hypoplastic pulmonary arteries, right ventricle–to–pulmonary artery (RV-PA) conduits (performed in repair of pulmonary atresia, truncus arteriosus, TGA with pulmonary stenosis [Rastelli procedure], some double-outlet right ventricle defects), and pulmonary hypertension. Conduits calcify and narrow, and together with the increasing stroke volume that occurs with growth, significant obstruction can develop. The septal shift associated with severe right ventricular pressure overload can compromise left ventricular function via a reduction in left ventricular filling and systemic outflow obstruction.
Hypoxemia and Cyanosis
Cyanosis is associated with decreased pulmonary blood flow or intracardiac mixing lesions, or both. Prior to repair, cyanotic lesions include tricuspid atresia, pulmonary atresia, tetralogy of Fallot, transposition of the great arteries, and truncus arteriosus; tricuspid atresia, pulmonary atresia, and TOF are all lesions that typically have reduced PBF. Increased PBF occurs in truncus arteriosus. In lesions with intracardiac mixing (e.g., TGA), cyanosis can occur with decreased or increased PBF depending on whether there is obstruction to the PBF. Cyanosis may also be found in the setting of very low cardiac output, increased arteriovenous oxygen difference, and respiratory disease. With the advent of early infant repair, chronic hypoxemia is now most frequently encountered in the young child undergoing staged repair, and in the adult with unrepaired or palliated CHD. Indeed, one stimulus for early, definitive repair is to eliminate hypoxemia and the compensatory polycythemia, with its rheologic, neurologic, hemostatic, renal, and metabolic consequences. Although the analyses are limited and imperfect for obvious reasons, the data that does exist suggests that chronic hypoxemia during infancy and early childhood is a significant risk factor for reduced cognitive performance. As blood viscosity increases, systemic (including coronary) and pulmonary vascular resistances increase markedly. Hemostatic abnormalities that can result from cyanosis and polycythemia include thrombocytopenia, platelet dysfunction, shortened platelet survival, disseminated intravascular coagulation, decreased production of coagulation factors, and primary fibrinolysis (Tempe and Virmani, 2002; Odegard et al., 2003, 2009). Sludging of red blood cells increases the risk for thromboembolism and stroke, particularly when the hemoglobin approaches or exceeds, 20 g/dL, and in conjunction with dehydration. Phlebotomy regimens are being used less frequently in the absence of symptoms, as they may be associated with an increased risk for cerebrovascular events (Ammash and Warnes, 1996). The duration and degree of hypoxemia and polycythemia are important historical factors in the evaluation of possible long-term residual cardiac muscle blood flow abnormalities.
Rhythm and Conduction Abnormalities
Arrhythmias and conduction defects have a major impact on the prognosis and management of patients who have undergone palliation or repair of CHD (Warnes and Deanfield, 2001). Rhythm disturbances that may be well tolerated in a structurally normal heart may be life threatening in a structurally or functionally abnormal heart. The etiology is multifactorial and includes damage to the arterial supply or direct injury to the sinoatrial node, atrioventricular (AV) node, and conduction system, atrial or ventricular scarring, chamber dilation or hypertrophy with resultant pathologic remodeling, and myocardial ischemia.
Arrhythmias may occur in the postoperative period or many years after surgery, and they tend to vary with the type of underlying heart disease and surgical procedures that have been performed (Vetter, 1991). Supraventricular tachycardias (atrial flutter/intraatrial reentrant tachycardia, atrial fibrillation) and sinoatrial node dysfunction (bradycardia, tachy-brady syndrome, exit block, sinus arrest) are more common in lesions that required extensive intraatrial surgery or have residual elevations in right atrial pressure, such as the atrial switch (Mustard or Senning) procedure for TGA, the Fontan procedure, and TOF repair. Isolated right bundle branch block is frequent after ventriculotomy. The QRS duration may be an independent predictor of arrhythmia, right ventricular dysfunction, and sudden death risk in patients after TOF repair (Gatzoulis et al., 2000a). Whether aberrant conduction and ventricular dyssynchrony are independent causes of ventricular dysfunction and, consequently, whether using biventricular pacing to restore normal activation-contraction patterns can prevent or reverse ventricular function in patients with dyssynchrony is currently under investigation (Cecchin et al., 2009). Ventricular arrhythmias are more common in lesions with residual ventricular pressure or volume load, as in aortic stenosis, hypertrophic cardiomyopathy, and TOF repair. Tachyarrhythmias and ventricular dysfunction are a dangerous combination and a cause of late sudden death (Vetter, 1991).
Existing pacemakers should be checked preoperatively and the appropriate precautions taken in patients with complete AV block. There is the need for preoperative evaluation and temporary resetting or shutting down of pacemakers and implantable cardioverter defibrillators (Practice advisory, 2005), as well as backup pacing (transcutaneous pacing) in the event of pacemaker malfunction. For high-risk patients, an external pacing or defibrillator unit should be in the operating room and pads applied around the time of induction of anesthesia. The need for and use of electrocautery (monopolar versus bipolar) in pacemaker-dependent patients should be discussed with both the surgeon and electrophysiologist. Implanted pacemakers and cardioverter defibrillators typically need to be interrogated and reprogrammed after the surgical procedure. The electrophysiologist may also be helpful for patient optimization. For example, consideration should be given to temporary pacing in select unpaced patients with bradycardia, as well as to radiofrequency catheter ablation in patients with amenable tachyarrhythmias, especially before major procedures.
Pulmonary Hypertension
In the unrepaired child, unrestricted left-to-right shunting with increased pulmonary blood flow produces a volume load on the heart and structural changes in the pulmonary vascular bed (medial hypertrophy progressing to necrotizing arteritis [Heath and Edwards, 1958]), leading to decreased myocardial function and pulmonary hypertension (mean PAP greater than 25 mm Hg). The time course for developing PVOD depends on the size and site of the shunt and age at surgery. Progression is more rapid when both the volume and the pressure load on the pulmonary circulation are increased, such as with a large VSD. For the majority of infants with an unrestrictive shunt, repair of the defect in the first year of life is usually associated with regression of the pulmonary vascular changes. Pulmonary hypertension develops more slowly with increased pulmonary blood flow in the absence of elevated pulmonary artery pressures, as with an ASD, where the absence of pulmonary hypertension into the third decade or beyond is not uncommon. Eisenmenger’s syndrome is characterized by irreversible PVOD and cyanosis related to reversal of the left-to-right shunt (Wood, 1958).
Anesthetic considerations: Severe pulmonary hypertension appears to impart major anesthetic risk, even for minor procedures (Ammash and Warnes, 1996; Raines et al., 1996; Daliento et al., 1998; Martin et al., 2002; Carmosino et al., 2007). This topic has been the subject of recent reviews (Subramaniam and Yared, 2007; Friesen and Williams, 2008). Suprasystemic pulmonary artery pressure is a significant predictor of major complications in children with pulmonary hypertension undergoing noncardiac surgery (Carmosino et al., 2007). It is not possible to recommend a specific anesthetic technique as all anesthetic techniques have been used successfully. Of note, many perioperative deaths occur in the postoperative period (Lyons et al., 1995; Martin et al., 2002). In older patients with Eisenmenger’s syndrome, most deaths appear to occur either as a result of the surgical procedure and not of anesthesia, or in the postoperative period because of complications such as atelectasis, pneumonia, worsening hypoxemia, or other end-organ dysfunction (Martin et al., 2002). Preoperative knowledge of the degree of pulmonary hypertension, pulmonary vascular reactivity, right ventricular dysfunction, and the presence of an intracardiac communication is imperative. For example, patients with severe pulmonary arterial hypertension, significant RV dysfunction, and no “pop-off” communication (i.e., right-to-left shunt) are probably the most at risk.
Acute right ventricular dysfunction and resultant low systemic cardiac output are the major pathophysiologic consequences of acute exacerbations in pulmonary artery pressure. The overall goals of anesthesia, therefore, are to provide adequate analgesia and anesthesia while minimizing increases in PVR and depression of myocardial function (Friesen and Williams, 2008). Likely methods include providing adequate preoperative sedation, high inspired oxygen, hyperventilation (respiratory alkalosis) if possible, adequate depth of anesthesia, maintenance of a normal to increased preload, early use of an inotrope to support RV function and systemic blood pressure (i.e., RV perfusion), and use of induction and maintenance agents that do not significantly reduce contractility or systemic blood pressure. Endotracheal intubation as a potential mechanical trigger of pulmonary vasoreactivity should be recognized; this also applies to extubation on emergence from anesthesia. In addition to adequate anesthetic depth, lidocaine spray to the vocal cords and trachea may offer some degree of protection. Noninvasive ventilation may be an attractive alternative to support adequate gas exchange during anesthesia and surgery under some conditions. Although allowing better control of oxygenation and ventilation, positive pressure ventilation increases RV afterload and decreases RV filling so that excessive inspiratory pressures and volumes, and positive end-expiratory pressure (PEEP), should be avoided. It is critical that pulmonary vasodilator therapy not be interrupted perioperatively, particularly prostacyclin (Flolan) infusions, whose discontinuation can result in severe rebound pulmonary hypertension in as little as 10 to 15 minutes. With severe pulmonary hypertension and known responsiveness of the pulmonary vasculature to NO, it is advisable to have NO available for immediate or even prophylactic administration. The use of invasive monitoring (e.g., arterial blood pressure) is usually determined by the nature of the surgical procedure. Because of the significant morbidity and mortality of anesthesia and surgery for the patient with severe pulmonary hypertension, a risk-benefit analysis involving the cardiologist, surgeon, and anesthesiologist is essential before performing elective procedures.
Infective Endocarditis
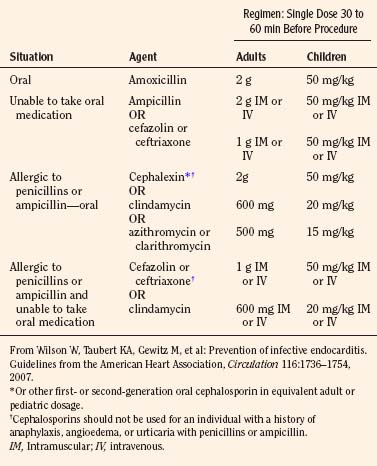
The most recent guidelines of the American Heart Association concluded that only an extremely small number of cases of infective endocarditis could be prevented by antibiotic prophylaxis for dental procedures (Wilson et al., 2007). As a result, infective endocarditis prophylaxis for dental procedures is recommended only for patients with underlying cardiac conditions (Box 21-2) associated with the highest occurrence and risk for adverse outcome from infective endocarditis. Prophylaxis in this group is recommended for all dental procedures that involve manipulation of gingival tissue or the periapical region of teeth or perforation of the oral mucosa. The antibiotic is administered in a single dose before the procedure (Table 21-1). Administration of antibiotics solely to prevent endocarditis is not recommended for patients who undergo a genitourinary or gastrointestinal tract procedure.
* Except for the conditions listed above, antibiotic prophylaxis is no longer recommended for any form of CHD.
† Prophylaxis is recommended because endothelialization of prosthetic material occurs within 6 months after the procedure.
From Wilson W, Taubert KA, Gewitz M, et al: Prevention of infective endocarditis. Guidelines from the American Heart Association, Circulation 116:1736–1754, 2007.
End-Organ Dysfunction and Injury
Unrestricted left-to-right shunting, in addition to increasing PAP and PVR, produces alterations in lung mechanics and airway compression. The primary effects on lung mechanics are a decrease in lung compliance and an increase in airway resistance (Bancalari et al., 1977; Stayer et al., 2004). Decreased compliance will necessitate higher than expected airway pressures, with care being taken not to insufflate the stomach during mask ventilation. Airway compression can result from dilated pulmonary arteries, left (or right) atrial dilation, massive cardiomegaly, or intraluminal bronchial obstruction (Berlinger et al., 1983). The pulmonary lymphatics are also compressed in these circumstances, perhaps explaining an increased incidence of pulmonary infectious symptoms in patients with large left-to-right shunts.
Neurologic injury and adverse neurodevelopmental outcome in CHD patients are multifactorial, with various contributions from genetic, lesion, and procedural elements (Newburger and Bellinger, 2006). Relatively pervasive issues include hyperactivity, diminished executive function, and various other neurocognitive abnormalities, especially in areas pertaining to speech and language and executive functions. Less commonly seen in the current era are seizures, stroke, and choreoathetosis. Structural brain abnormalities have been found with magnetic resonance imaging (MRI) in infants with CHD before any intervention, as well as after surgery or balloon atrial septostomy (Mahle et al., 2002; McQuillen et al., 2006; McQuillen et al., 2007; Miller et al., 2007; Andropoulos et al., 2010). Complex CHD may have anywhere from a mild to a profound impact on a child’s psychosocial development (Horner et al., 2000). These issues necessitate additional sensitivity with the family, altering the amount of detail discussed in front of the child when obtaining informed consent, and precluding certain sedation or regional anesthetic techniques.
Chronic cyanosis, low systemic cardiac output, or high venous pressures (Damman et al., 2009) may over time contribute to the development of renal and hepatic insufficiency. This may not be evident on routine laboratory tests (e.g., serum creatinine or liver enzymes) but may predispose to perioperative dysfunction in response to relatively minor changes in organ perfusion and oxygen delivery, or to otherwise relatively mild toxic stresses (e.g., ketorolac). Cardiac catheterization (contrast nephropathy) increases the risk for perioperative renal dysfunction (Briguori et al., 2007).
Extracardiac Anomalies
Extracardiac anomalies occur in 25% of infants seen during the first year of life in patients with cardiac disease (Greenwood et al., 1975). The anomalies are often multiple and may result from chromosomal, genetic, teratogenic, or unknown causes.
Heart Transplant Recipients
The worldwide annual transplant rate in children is around 400, with the major indications being cardiomyopathy and congenital heart disease (Kirk et al., 2008). Factors to consider in this population are cardiac physiology and functional status, cardiac allograft vasculopathy, rejection, the side effects of immunosuppressive agents, and the development of renal dysfunction, hypertension, and malignancy. Efferent denervation results in a resting tachycardia (withdrawal of vagal tone) and impaired chronotropic response to stress. Afferent denervation results in lack of angina during myocardial ischemia and alterations in cardiac baroreceptors and mechanoreceptors. Cardiac physiology is restrictive, with mildly elevated filling pressures and a low-normal ejection fraction (Cotts and Oren, 1997). There may be sinus node dysfunction and there is a shift from β1 to β2 receptors.
Anesthetic considerations (see Chapter 20, Anesthesia for Congenital Heart Surgery, for a more complete discussion): The response to hemodynamic instability is slower (dependence on circulating catecholamines) and less robust. The denervated heart is preload dependent, with a reduced chronotropic response to hypotension or sympathetic stimulation. Restrictive physiology, particularly with rejection, increases the risk for pulmonary edema when fluid administration is not judicious. Sensitivity is increased to direct-acting catecholamines, β-blockers, adenosine, and verapamil, and it is decreased to digoxin and indirect-acting sympathomimetic agents. Myocardial ischemia is an ever-present threat from coronary artery vasculopathy. A new onset of dysrhythmias or heart block is ominous, suggesting rejection or myocardial ischemia. Immunosuppression requires strict aseptic technique, and the hypertension and nephrotoxicity associated with some agents and possible need for stress-dose corticosteroids need to be addressed.
Preoperative assessment
CHD adds significant risk for morbidity and mortality in patients requiring noncardiac surgery (Warner et al., 1998; Coran et al., 1999; Baum et al., 2000; Martin et al., 2002; Carmosino et al., 2007). The preoperative evaluation should be complete enough to provide a clear understanding of the pathophysiology of the cardiac defect, the implications of any corrective or palliative procedures, and the likely interactions with the planned surgical procedure. As a general rule, patients with CHD who are doing well clinically (i.e., have good functional status, few or no medications, and only routine medical examinations) tend to do well with anesthesia and surgery. Not surprisingly, the unrepaired or palliated patient presents a greater risk, as does the more complex and stressful surgical procedure. Broadly speaking, there are three categories of patients with CHD: those who have undergone a reparative (corrective) procedure, those who have undergone a palliative procedure, and those who have not undergone any procedure. The principles of anesthetic management are the same whether the patient is a child or an adult, and whether they have had a procedure or not.
History and Physical Examination
As the history may be incomplete or misleading with complex CHD (Colman, 2003), close collaboration with the patient’s cardiologist is valuable. Additionally, the cardiologist can help identify patients at high risk, clarify pathophysiologic issues, establish if the current clinical status is the best possible, and provide the findings of recent cardiologic studies. The focus of the history should be on the type of lesion and factors listed in Box 21-1, prior surgical and catheterization procedures and complications thereof, anesthetic experience, medications, allergies, and current functional status. Specific symptoms that should be sought are feeding difficulties and sweating in infants, poor growth, cyanotic spells, decreased activity level such as inability to keep up with healthy peers, fatigue, dyspnea, palpitations, chest pain, and syncope. New or worsening symptoms require cardiology consultation. Recent respiratory tract infections can cause changes in pulmonary vascular resistance and airway reactivity, increasing anesthetic risk in the setting of decreased pulmonary compliance, pulmonary hypertension, systemic-to-pulmonary artery shunts, and cavopulmonary anastomosis.
The physical examination should include general appearance, level of activity, presence of distress, and vital signs. Arterial oxygen saturation (SpO2) varies with clinical status, but is expected to be above 94% after definitive procedures and in the range of 75% to 85% after palliative interventions that create shunted or intracardiac mixing circulations. Evidence of tachycardia, cyanosis, tachypnea, labored breathing, congestive heart failure, and poor peripheral perfusion should be sought. Airway assessment is important, because extracardiac anomalies may be present in up to one quarter of patients with CHD (Friedman, 1997). Peripheral pulses and four extremity blood pressures should be assessed in the setting of known or suspected aortic arch obstruction, previous or present Blalock-Taussig shunts, or after multiple cardiac catheterizations.
Special Investigations
The extent of laboratory testing depends on the child’s clinical status and the complexity of the planned procedure. General recommendations for blood testing include the following: (1) hematocrit or hemoglobin if the child is pale, cyanotic, or undergoing a procedure with the potential for significant blood loss; (2) serum electrolytes for patients with renal dysfunction or those receiving diuretics, angiotensin-converting enzyme inhibitors, or digoxin (although preoperative electrolyte disturbances in children and young adults presenting for cardiac surgery are uncommon [Hastings et al., 2008]); (3) platelet count and coagulation studies for cyanotic children or those on anticoagulants or antiplatelet agents; and (4) blood typing and cross-matching if significant blood loss is anticipated. A chest radiograph should be obtained with new cardiorespiratory symptoms or abnormal findings on clinical examination, or if dictated by the surgical procedure. Cardiologic studies should be coordinated with the child’s cardiologist, because some tests will have been recently completed, and investigations such as cardiac catheterization, Holter monitoring, exercise stress tests, and cardiac MRI mandate the cardiologist’s input. The electrocardiogram is reviewed for rhythm abnormalities, impaired conduction, chamber enlargement, and ischemia. Changes from prior studies need to be explained before proceeding. Preoperative consultation with the cardiologist is essential for patients with pacemakers, with evaluation of the pacemaker and a clear plan made for appropriate adjustment on the day of surgery (see earlier) (Practice advisory, 2005). In all but the simplest lesions, recent echocardiography is probably useful to document the current status of anatomy and ventricular function.
Procedure Scheduling
Institutional practices vary in the provision of anesthetic care for the highest-risk children with CHD. The aging of the CHD population has also resulted in adults with CHD undergoing noncardiac procedures at pediatric institutions (Warnes et al., 2001). In some institutions, anesthesia is provided by those who routinely practice pediatric cardiac anesthesia, and in others (including our own) pediatric anesthesiologists who do not practice cardiac anesthesia provide the care (Walker et al., 2009). The important point is that the case be assigned to an anesthesiologist who will understand the cardiac pathophysiology and know how to prevent and promptly deal with cardiac-related complications.
Intraoperative management
Premedication
Midazolam, 0.5 to 0.75 mg/kg orally, is usually sufficient, but for patients who have had multiple surgeries and catheterizations and thus are likely to be more anxious and perhaps more tolerant to sedative medications, it is often necessary to increase the dose to 1 mg/kg (Masue et al., 2003); sometimes oral ketamine, 3 to 10 mg/kg, is added as well (Auden et al., 2000; Funk, et al., 2000). Troublesome ketamine-stimulated secretions can usually be controlled with glycopyrrolate once intravenous access is established. If the patient has intravenous access in situ or after placement, a small bolus of midazolam, 0.05 mg/kg, repeated as necessary, will provide anxiolysis and facilitate separation from the parents. Intramuscular sedation with ketamine, 3 to 5 mg/kg, with or without midazolam, 0.05 to 0.1 mg/kg, may be necessary for the uncooperative or combative child who will not accept oral premedication and for whom an intravenous induction is most desirable. A combination of oral meperidine and pentobarbital for heavy premedication of CHD patients has been used with a substantial track record of safety and success (Nicolson et al., 1989), but insufficient effect and rage-like reactions (most likely attributable to pentobarbital) are known side effects. After any heavy premedication, the anesthesiologist should remain with the patient, and, particularly for patients with cyanotic CHD, oxygen saturation should be monitored and oxygen administered as needed (Stow et al., 1988; DeBock et al., 1990).