Chapter 18 Blind Digital Intubation
I History
Although it was probably first described by Herholdt and Rafn in 1796 for the management of drowning victims,1 blind digital orotracheal intubation did not receive much attention in the medical literature until its revival in emergency medicine and prehospital care by Stewart in the mid-1980s.2,3 Notable publications over the years have portrayed the technique as an acceptable, if not preferable, alternative to standard laryngoscopic endotracheal intubation, particularly when the standard technique is contraindicated, has failed, or is not possible because of a lack of equipment.
In 1880, Macewen described the technique utilizing a curved metal tube in awake patients,4 and Sykes5 recommended routine use of the digital technique in anesthetic practice in the 1930s. Siddall and Lanham relegated the technique to last-ditch efforts following the failure of conventional intubation methods.3,6,7 The technique has been described in neonatal resuscitation and as an adjunct in blind nasotracheal intubation.8–10
Currently, there is widespread variation in awareness, expertise, and application of the technique in anesthesia, emergency medicine,11,12 and prehospital care. Although advances in airway management equipment and expertise have made obsolete the routine use of blind digital orotracheal intubation, it remains a valuable skill in some situations, especially in the emergency setting or under circumstances in which the anesthesiologist cannot be positioned at the head of the patient,3 rendering laryngoscopic intubation impossible.
II Indications
1. When equipment required to undertake alternative techniques is unavailable or not functional.
2. When positioning of the patient or the anesthesiologist prevents conventional intubation.
3. When other methods have failed or are likely to fail and the skill and experience of the anesthesiologist make the digital technique a reasonable alternative.
4. In the presence of potential or actual cervical spine instability when the anesthesiologist selects the digital technique on the basis of the risk-benefit analysis. Although there is no evidence to suggest that the use of digital intubation alters the neurologic outcome of a patient, there may be less cervical spine motion during intubation with the digital technique compared with conventional laryngoscopic orotracheal intubation without in-line stabilization.
5. When adequate visualization of the airway to allow conventional intubation is not possible because of the presence of copious secretions, blood, or vomitus in the oropharynx or traumatic disruption of the upper airway anatomy.
III Technique of Digital Intubation
A Preparation
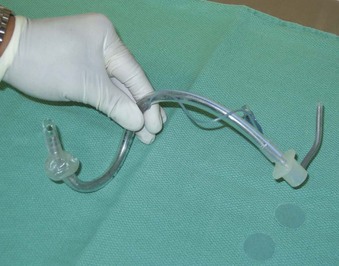
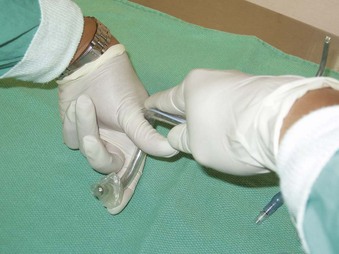
As with any intubation technique, preparation involves assembling the necessary equipment and personnel, including emergency drugs and adequate suction, to optimize success and preserve ventilation and oxygenation. An appropriately sized ETT is selected. The use of a stiff but malleable stylet improves maneuverability during the intubation. Lubrication of the stylet with a water-soluble lubricant ensures easy retraction after the tip of the ETT is placed in the glottic opening. The stylet is then inserted into the ETT so that the distal end of the stylet is at the level of the Murphy eye. With the stylet in place, the distal half of the styletted ETT unit (SETT) is bent into a “U” configuration (Fig. 18-1). The proximal half of the SETT is then bent approximately 90 degrees toward the dominant side of the ETT to allow manipulation of the SETT by the dominant hand during intubation (Figs. 18-2 and 18-3). The degree of bend should be individualized and is dependent on the anesthesiologist’s experience.
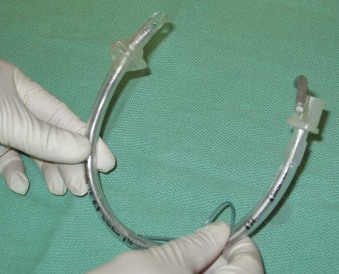
Figure 18-1 With the stylet in place, the distal half of the endotracheal tube is bent to a U shape.
C Technique
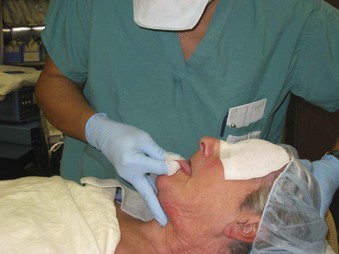
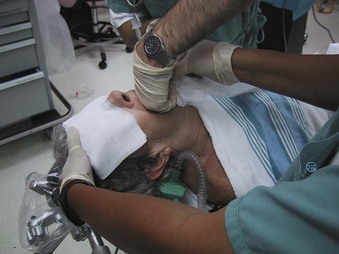
Pulling the tongue forward by an assistant facilitates palpation of the epiglottis, thus improving the success rate for digital intubation. The patient’s mouth is opened, and the tongue is grasped gently by the assistant with a piece of gauze (Fig. 18-4). Traction on the tongue moves the epiglottis slightly cephalad, enhancing its palpability and facilitating placement of the tip of the ETT into the glottic opening. The anesthesiologist then inserts the index and middle fingers of the nondominant hand into the oral cavity and slides the palm down along the surface of the tongue (Fig. 18-5). The tip of the middle finger touches the tip of the epiglottis, which is then directed anteriorly (Fig. 18-6). The ease of palpating and lifting the epiglottis depends on the length of the anesthesiologist’s fingers, the height of the patient, the anatomy of the oropharynx, and the presence or absence of teeth.

Full access? Get Clinical Tree